PACE-CME
Subtitles available: Italian, English, French & more
Why is early screening and risk identification of CKD in diabetes important?
Dear colleagues. I'm glad to be here today to talk a little bit about early screening and risk identification in chronic kidney disease in patients with diabetes and why this is so important. These are my disclosures.
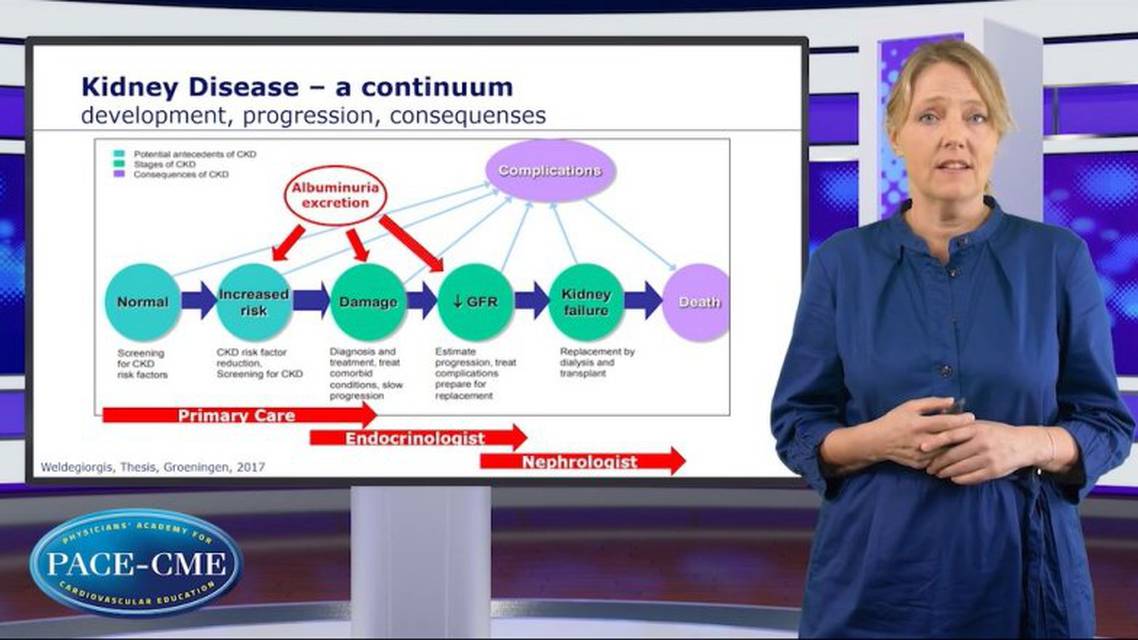
So, as with many other chronic diseases, kidney disease can be seen as a continuum with a large group in the beginning of increased risk and ending up in the more end state events like, dialysis, kidney transplantation and increased mortality, especially due to cardiovascular mortality. But actually, in the years before this, many patients would have gone through years with a steady decline in kidney function, measured by GFR or eGFR. And also, we know that in the early stages, albuminuria can be a strong marker of the patients that you have to take extra care of, that are in the high risk. However, the patients at this stage will not be in the nephrology care, they will be taken care of in the primary care. And also when signs of the complications of the diabetes shows, they will be in the diabetologist's, endocrinologist's care. First, at a late stage, the nephrologist will enter the scene. And at this point, actually, a lot of focus will be on the medical challenges, secondary to kidney disease and also getting a planned dialysis start and so on. So it's clear if we need preventive measures and intervention, this will have to be a collaboration between the specialties. ‘
We know from much evidence that moderately increased albuminuria also called microalbuminuria, with an albumin creatinine ratio above 30 and less than 300 milligrams per gram, predicts the development of diabetic nephropathy. It also predicts the prevalence of the other diabetic complications and it's correlated closely to cardiovascular morbidity and also mortality, both all-cause and especially cardiovascular mortality. It has a significant correlation to blood pressure and blood pressure control but albuminuria is not just a sign of the kidney having damage from these metabolic changes. It is thought of as a widespread endothelial dysfunction marker.
Many other markers have been proposed for identifying the high-risk population who will develop these different pathophysiological stages. You can see at the bottom for diabetes nephrology. And we hope one day to have a pattern or a marker that can precisely identify the patients that we have to look at. But for now actually, our strongest marker is the urinary albumin creatinine ratio. This is a non-invasive measure in a substance that patients have to get rid of anyway, so it should be able to be accessible.
We know, for instance, from studies like this where 15,000 participants with type 2 diabetes were analyzed for the 10-year mortality, that when you categorize your patients by kidney status, namely by albuminuria, above 30 milligrams per gram or impaired GFR, here below 60 milliliters per minute, or combined, you can see that the dotted line is the general population and everything above the dotted line will then be excess mortality. And you can see the strong markers, how strong the markers of kidney disease are. Actually, the authors of this paper concluded that those with kidney disease are predominantly accounting for the increased mortality in type 2 diabetes.
So, what have we done to change the course of diabetic nephropathy because we have done a lot in the last 30 years. I think two important things can be said, systematic screening and preventive treatments. So the success story lies within this and I think we have over the last years, really seen that preventive treatment is available. Some of the data and there's of course a lot of studies but some of the data is naturally the aggressive treatment of blood pressure and also inhibiting the renin-angiotensin system.
Here you can see the irbesartan trial in type 2 diabetes with microalbuminuria and the effect of RAS inhibiting on progressing to nephropathy. This is just one of many studies.
Also, we know that the multifactorial approach is very important. Here is the Steno2 Study from the 90s at the Steno diabetes center in Copenhagen. A rather small study that many of you would have heard about. 80 patients. Typical type 2, middle-aged patients with microalbuminuria randomized to conventional therapy at the general practice, which was really not very intensive in the 90s. Or intensive care at the Steno Diabetes Center where approach was on very ambitious goals. Aggressive drug treatments with exactly RAAS inhibition, statins, aspirin and ambitious goals for blood pressure. But on top of this, there was a proactive behaviour modelling and a continued patient education motivation. So in 2016, we got results: the 21-year data. Actually, at this point half of the cohort had passed. We could see that from this intensive intervention in the beginning of the study actually almost eight years of life was gained. That's quite impressive. When we looked at the earlier data on the combined end stage renal disease and death, there was also a significant reduced risk of almost half. So it's no wonder that these are the studies that are behind our standard of care today.
We've seen it as well with all the other complications, that our systematic, screening and preventive measures are what have turned the life around for many individuals with diabetes.
So, how are we doing? I found this new study from the US. These are 24 primary care organisations. What they examined was the electronic records of 500,000 type 2 diabetes patients. On annual albumin creatinine ratio testing. The mean was actually 53 percent. Even though, it was seen that the eGFR measuring was much higher.
But what is interesting to see, is when you look at the clinical practice site you can see that a lot of sites actually have the testing down probably to a standard daily care. Whereas, at the bottom, there are practice sites that might have not gotten the focus on urinal testing or they might be testing in a way that doesn't show up in the electronic journals. We can hope that.
Similar data are available from Denmark where we looked at three cross-sectional studies in general practice in Denmark from 2012 and 2016 to 2020. We can see an improvement in the annual albuminuria measuring from 57 up to 82 percent. So this is good news and I'm convinced that this is exactly due to the systematic screening. The way that it has improved is by having a large focus on the type 2 diabetes disease and being educated. Also, the government doctor agreements on reimbursement probably had some weight.
So, the importance for this measurement is that actually for the treatment of type 2 diabetes, in the new changing international diabetes guidelines, we need this early on, we need to categorize our patients.
Up here, after starting metformin and giving lifestyle advice, you can see that we have to categorize the patient that has ischemic heart disease, signs of chronic kidney disease or heart failure. This is independent of baseline A1C, meaning this is actually not only hyperglycemia treatment, but actually going in a perspective of more organ protection as you've heard over the last years.
So, just to run you through some of the large studies that changed the guidelines, some of them will be very familiar to you. It all started in 2015 in Stockholm where the SGLT2 inhibitor empagliflozin was examined over placebo. It was the EMPA-REG trial and it gave us very interesting and positive results with in cardiovascular disease and also mortality. In this group of patients with type 2 diabetes and very high or prior cardiovascular disease. But already at this point, we also saw that a kind of mixed combined renal endpoint also seemed to really benefit from the SGLT2 inhibitor treatment. We've seen more of these effects over the last years and we also wait for empagliflozin in a real kidney cohort. The EMPA-KIDNEY trial will be coming out with results maybe later this year.
At the same conference, actually, the LEADER trial was presented. This is the GLP-1 receptor agonist liraglutide and this also showed really great benefit in cardiovascular end points in type 2 diabetes. But also here we saw a sign of this combined renal endpoint having a good effect of GLP-1 receptor agonist treatment. And we will look very much forward to the renal trial, with this agent actually, the FLOW trial, which will be giving out results in some years.
Then came the CREDENCE trial to show that SGLT2 is a strong treatment into the lower GFR areas of type 2 diabetes. And in 2020 we had the DAPA CKD trial which went even further down in GFR. Two things were really important from the DAPA CKD trial. Trying it out on patients with low GFR, where it was safe and effective. And also that one third of the patients in this more than 4,000 patient group actually was without diabetes. And we didn't know whether this would actually be effectful when we didn't have hyperglycemia and everything in the re-uptake inhibition in the kidney. But as you can see here, on all outcomes, the primary and some of the renal and cardiovascular outcome, both type 2 diabetes and non diabetes CKD, had a great effect on dapagliflozin. Changing guidelines as we speak actually, and also the all-cause mortality was quite convincing.
So I found an old quote that we have seen before. It's from 1976, and it states that diabetic nephropathy is an irreversible disease with no cases of recovery and once the clinical signs of nephropathy can be seen it's downhill from there with an accelerated progression in the later stages. I think we've come a long way and it is also almost 50 years.
If we look at diabetic kidney disease today and look at the slope of the yearly GFR decline, we know that an untreated hypertensive diabetic kidney disease patient can lose more than 12 ml per minute per 1.73 standard square meters every year. And we know that when we aggressively treat this with antihypertensive treatment and RAS inhibition, we can get that down to a decline from three to five ml per minute. Try and have a look at the placebo groups here of the big SGLT2 trials, CREDENCE trial, with type 2 diabetes with signs of nephropathy. A decline of 4.6 ml per minute, every year. EMPEROR-Reduced, empagliflozin in a heart failure cohort, not a kidney disease cohort. A decline of 2.3 mL per minute, every year. And finally, the DAPA CKD, where the mean GFR was 43 mL per minute. So quite a kidney-sick cohort and decline of 3.6 mL per liter. And adding SGLT2 treatment to these groups, you can see the fine results in helping these people having much less decline every year. Meaning longer time to dialysis longer time to end stage renal disease. So we have come a long way.
So my take home messages today. Change in kidney disease happens early. In primary care, use the tools for systematic approach. That can be the digital tools you have available. May I say that nurses are also very good at a systematic approach, so use them if you have the possibility there. Discuss in your local setting who is responsible for what. The endocrinologist, cardiologist, the nephrologist. Focus on guideline recommended annually albuminuria measurements. It is a reliable marker. It can predict high risk individuals who are in need of organ protection, and this modern diabetes treatment, and it can also guide your treatment to see if you're doing well, or if you need to be more aggressive. And then I think we should consider whether this systematic approach that we have been using in diabetes, might be the same way to go for the non-diabetic chronic kidney disease patients. So lots to do. Thank you.
Recommended
- Primary care as gatekeeper in CKD and the need for collaboration with nephrologistsPrimary care as gatekeeper in CKD and the need for collaboration with nephrologistsRethinking the role of nephrologists in prevention of CKD - The opportunity of early risk identificationPrimary care as gatekeeper in CKD and the need for collaboration with nephrologists
- Discussion - Rethinking the role of nephrologists in prevention of CKD - The opportunity of early risk identificationDiscussion - Rethinking the role of nephrologists in prevention of CKD - The opportunity of early risk identificationRethinking the role of nephrologists in prevention of CKD - The opportunity of early risk identificationDiscussion - Rethinking the role of nephrologists in prevention of CKD - The opportunity of early risk identification
- Barriers for preventing CKD in patients with diabetesBarriers for preventing CKD in patients with diabetesRethinking the role of nephrologists in prevention of CKD - The opportunity of early risk identificationBarriers for preventing CKD in patients with diabetes







