PACE-CME
Subtitles available: English, French, German & more
Primary care as gatekeeper in CKD and the need for collaboration with nephrologists
Thank you very much for joining me today in this presentation 'Primary Care as gatekeeper in chronic kidney disease: The need for collaboration with nephrologists.' These are my disclosures.
As we know the prevalence of chronic kidney disease is increasing. In 1990, it was ranked 17th most common cause for global mortality. In 2017, it was the 12th most common cause of global mortality. And we know the estimated prevalence of CKD globally is around nine percent obviously varying between different countries. But we still have a huge number of people who are undiagnosed and these are mainly in the early asymptomatic stages. The leading causes of CKD, as you all know, are diabetes and hypertension. We will come to that a little bit later on.
Type 2 diabetes and CKD drive a number of vascular risk factors. If you look at this, there is hypertension, CKD, type 2 diabetes, chronic heart failure, and cardiovascular disease. They are all interlinked in some way. And the reason is some of the pathophysiological mechanisms driving these conditions are shared between all of these chronic conditions.
Currently we work in an environment where we talk about type 2 diabetes, CKD, heart disease, heart failure. And they often see four or five specialists if they have all these conditions. We really need to move away from this one condition, one patient mentality to looking at these people more holistically because we know that they are interlinked.
We will show you some data that most people with one of those conditions will have other conditions as well. In terms of diabetes, we know that the risk factors are hypertension, age, family history and this puts people at increased risk. Following this, as we go along the pathway for diabetes and as we get to increased number of years of diabetes we will start getting complications such as albuminuria coronary artery disease and left ventricle hypertrophy. Then further progression occurs in terms of reduction in eGFR and cardiovascular events. And later on, down the line, we go to the end stage kidney failure and sometimes end stage heart failure as well.
Now this is a really key slide from a very recent study showing that CKD is a multimorbid condition. So at the top, you can see the concurrent conditions that are present in people with CKD. This is a large Scottish primary care database. As you can see, hypertension is four times more likely in people with CKD, heart failure diabetes, coronary heart disease, peripheral arterial disease, atrial fibrillation, stroke and transient ischemic conditions. But we look down below and there are other nonconcordant conditions such as liver disease, rheumatological conditions, inflammatory bowel disease and chronic obstructive airway disease. So these people have a lot more conditions then just CKD and it is similar for diabetes as well.
The same large study of over a million people is looking at adjusted odds ratio for people with CKD, comparing them to people without CKD. And as we can see, if they have one condition one comorbidity they're more likely to have CKD and the adjusted odds ratio is 6.5. If they have two or three chronic conditions, the adjusted odds ratio is 15. And if they have seven or more conditions and there are about 11 percent of people who have seven or more conditions the adjusted odds ratio for CKD is about 41. So CKD is a multimorbid condition or a multiple long-term condition.
We need to talk about COVID in these times as well. This is a systematic review and meta-analysis we conducted. When COVID came through, we thought it was a respiratory condition. However, as we can see from this meta-analysis are the cardiometabolic and renal conditions that are predominantly affecting people with COVID and giving them worse outcomes. This is the pooled rate of mortality in people with COVID-19 and comorbidities. Hypertension, diabetes, cardiovascular disease, CKD, cerebrovascular disease, these are the predominant conditions, as well as COPD and cancer.
So coming back to CKD, most cases are cardiometabolic in nature. And the KDIGO guidelines, which I have the pleasure of being on recommend screening for CKD in individuals with diabetes, cardiovascular disease and hypertension. As you can see about 42 percent of people with CKD have diabetes and about 17 percent have hypertension.
And we know there are differences in how primary care manages CKD and how nephrologists manage CKD. This is an old, but quite relevant study. They looked at the influence of early referral to a nephrologist on kidney function decline in patients with diabetes and CKD. As you can see on the left-hand side, the nephrologist care, about 52 patients. On the right-hand side, primary based care, 65 people. In terms of age, duration of diabetes and duration of hypertension, are similar. If you look at the baseline and final improvements in outcomes for systolic blood pressure, we see reduction in systolic blood pressure in nephrologist care but we don't see such an impact, in fact a possibly worsening of blood pressure in those who were under primary care. We see that albuminuria and eGFR do decline under nephrologist care and that is inevitable in people with chronic kidney disease. On the right-hand side in primary care, it gets a lot worse and the decline for eGFR is also worse. The proportion of patients who are on protective therapies such as ACE inhibitors or ARB, statins, is much higher in the final data for nephrologist care and very little change for some of the therapies under primary care. Finally, if we look at use of non-steroidal anti-inflammatory drugs that could give more damage in people with CKD none of the patients who were on this were under the nephrologist care. In terms of primary care there was an increase in nonsteroidal anti-inflammatory therapies in patients in primary care.
We also look at people here in early nephropathy or overt nephropathy. And again there doesn't seem to be much distinction in primary care in the patients who have early nephropathy or overt nephropathy. In fact, people with overt nephropathy get a lot worse in terms of blood pressure management and albuminuria is significantly worse as well. While on the left-hand side, people who have early nephropathy and overt nephropathy they seem to be well managed particularly when we look at their blood pressure management.
Another important aspect is: do people with CKD know they have CKD? This is a problem that we see regularly in primary care. For example, when patients get a letter to take part in a CKD studies and we've seen this in my own practice, because they've had an eGFR they've been picked up for a trial and they get a letter to say you have chronic kidney disease, but patients don't know they have that and they really get irate about this. And this is, again, a study conducted a few years back, looking at patient-reported care by different specialities between 2000 and 2007. As you can see CKD stages one and two and then CKD stages three to five. People under primary care, people with and without diabetes around 60 percent will be managed there for CKD stage one and two and CKD stages three to five. Internists about 17 percent with diabetes, 14 percent with no diabetes. But in terms of CKD three to five much further down the line, more patients were under internists. And as you can see a small proportion of people being managed by nephrologists across all CKD stages. However, when you look at the patient-reported care for CKD patients and whether they were aware of the disease you can see that not many people were aware under primary care. Even with CKD stages three to five only 66 percent were aware. Under internists about 22 percent were unaware and nephrologists about 2.3 percent were unaware. Under nephrology obviously a lot more people seem to know because they have been referred to a nephrologist.
In terms of management I think we need to take a holistic approach. This is from the KDIGO guidelines. The most recent one we published. And we need to think about our chronic care model. There are a number of examples of chronic care models. So you need a health system organisation of CKD care. So you need self-management support, a delivery system design, clinical information systems, computer systems which have a decision support as well. Within the community, you need the resources and the policies in place such as guidelines. As well as that, you need a prepared, proactive multidisciplinary team as well as an informed patient who is empowered. So they have the knowledge to manage their disease. All of these together with productive interactions between the multidisciplinary team and the activated patient should lead to improved outcomes. There are studies to show that as well.
As I said, now that CKD is a multi morbid condition, we need to approach this differently. We have CKD, we have CVD, we have diabetes. What we call the cardio-renal syndrome. And we really now need to approach this more holistically particularly in primary care. Because of as I said, the shared risk factors: age, hypertension, dyslipidemia and obesity.
And let's just go through what we have done in diabetes because there is a lot to learn from there that we can take into CKD as well. Remember, the prevalence of diabetes is around 6 to 8 percent globally, while for CKD we showed that the prevalence is around 9 percent or even higher because many people don't know it. But if you look at this, about 20 years ago around 60 percent of people with diabetes were managed in a primary care setting. About 25 percent in a shared care and about 12 percent in a secondary care setting. And we used to run our surgeries from these type of small practices.
But now we have much larger practices, multidisciplinary teams and this is the case for many developed countries. The new models of care, about 95 percent of people with diabetes are being managed in primary care and about 5 percent in secondary care. And how did we do this?
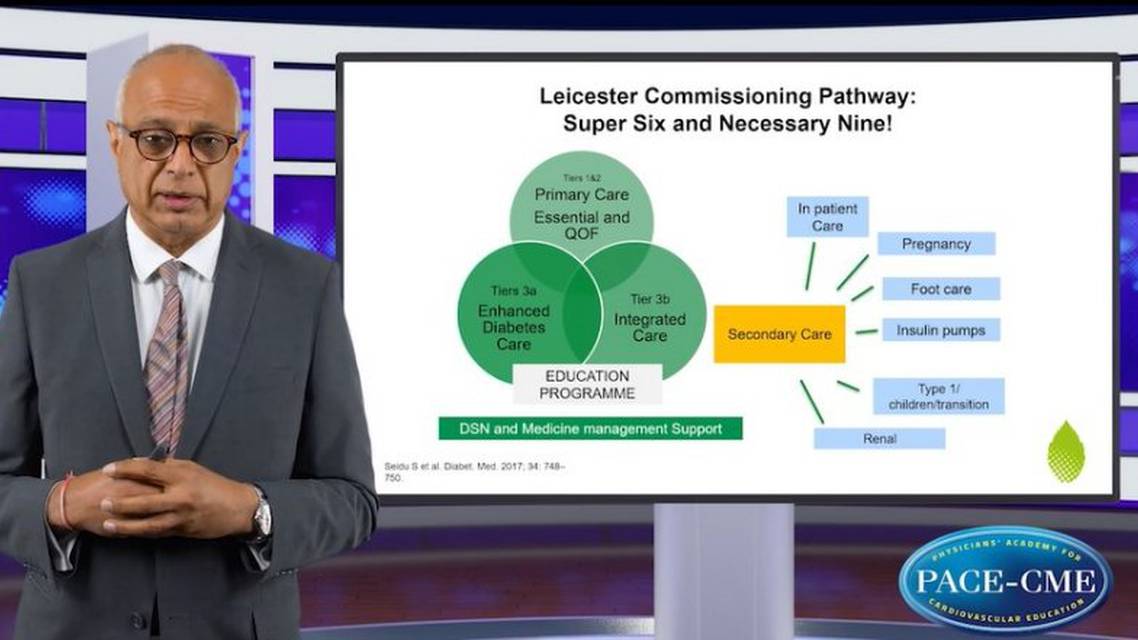
Well, this is one of our models from the UK in Leicester. What we really need to do is have an education program in collaboration with diabetes. This is what we did here, and we need to do this for CKD in a collaboration with our nephrology colleagues. So we have different tier systems, depending on how prepared the practices are. There is a medicine management support with the nurses and the general practitioners. But an ongoing education program. This is the evidence for CKD, diabetes, cardiovascular disease, is moving at pace. It's not just a one-off education program. This is an ongoing program, empowering healthcare professionals to manage people with these chronic conditions adequately. Then we have a secondary care who manage patients and these are what we call Super Six patients. So these are in-patient care, pregnancy, foot care, insulin pumps, type 1 diabetes in children and renal disease. More specialistic. This is when we would refer patients from primary care to secondary care colleagues. This is not the end of the road for those patients. We don't just hand them over to secondary care. When secondary care feels they are properly managed and they could be sent back to primary care we will continue looking after them in primary care. And when the time is right and if there develop further complications we can refer them to a secondary care colleague.
So, what we need to do, is think about fragmentation of CKD care. Most patients are managed in primary care or secondary care. It's pretty haphazard, like it was in diabetes. And we really need to think about a collaborative integrated approach where primary care and specialist care are working together to manage CKD. Where is it most appropriate to manage these patients? Is it primary care or is it secondary care? Move patients around is appropriate when needed to do this.
We have a multidisciplinary model of care for people with diabetes. As you can see a number of people involved. The person with diabetes is at the center. Then there's the general practitioner, the diabetes specialist nurse, the pharmacist. We have healthcare assistants. We have remote access to diabetes specialists. As well as that, people with diabetes get complications, cardiologists nephrologists, psychologists. They're also involved and podiatrist. There's no reason why we cannot develop a similar model of care for CKD with a person with CKD being in the middle with that multidisciplinary team around them.
In integrated care, the key to management is patient engagement, education and activation. And this also includes a use of new technologies that are coming. Home blood pressure monitoring is coming. We are using CGM for our patients. We also, as I mentioned we need to empower our healthcare professionals in primary care. We need to break down these speciality barriers, integration of medical workforce. Training needs to be done as well. If we empower our healthcare professionals and patients in a primary care setting, we can adequately look after them, like we have done in diabetes. Now with COVID, we've got new ways of working. So, patients don't need to go to specialist care. We have virtual clinics. We're also getting new specialists who are cardio-renal-diabetologist specialists. These people are also becoming specialists in primary care. We have what is called GP's with a special interest in various diseases.
So now, we need to start thinking about new models of care. And this is the time to start thinking about some of the questions. What are the variations in outcomes of people with CKD in primary care? What patient population should be referred to a nephrologist? Might the availability of new treatments for CKD change the referral pattern or would this be the least desirable in some cases? We can manage most of these patients in primary care. All the new therapies that are coming are easily manageable in primary care and prescribable in a primary care setting. As long as we have got empowered primary care practitioners. What could be powerful measures to improve the primary care physician-nephrologist interaction in CKD patients? And really, we need to think about what does a good integrated model of care for people with CKD look like? And move towards that model of care. Thank you very much for listening.
Recommended
- Discussion - Rethinking the role of nephrologists in prevention of CKD - The opportunity of early risk identificationDiscussion - Rethinking the role of nephrologists in prevention of CKD - The opportunity of early risk identificationRethinking the role of nephrologists in prevention of CKD - The opportunity of early risk identificationDiscussion - Rethinking the role of nephrologists in prevention of CKD - The opportunity of early risk identification
- Why is early screening and risk identification of CKD in diabetes important?Why is early screening and risk identification of CKD in diabetes important?Rethinking the role of nephrologists in prevention of CKD - The opportunity of early risk identificationWhy is early screening and risk identification of CKD in diabetes important?
- Barriers for preventing CKD in patients with diabetesBarriers for preventing CKD in patients with diabetesRethinking the role of nephrologists in prevention of CKD - The opportunity of early risk identificationBarriers for preventing CKD in patients with diabetes







