Statin use and risk of intracerebral hemorrhage
17/05/2012
This study examined the risk of hemorrhagic stroke in patients treated with statins, evaluated the effect of statins on total stroke and all-cause mortality, and determined whether hemorrhagic stroke was related to change in LDL-cholesterol. All available RCTs of statin therapy reporting hemorrhagic stroke rate were included in a meta-analysis.
A Meta-Analysis of 31 Randomized Controlled TrialsLiterature - McKinney JS et al, Stroke 2012 , May 15
Statin Therapy and the Risk of Intracerebral Hemorrhage :
McKinney JS, Kostis WJ.
Stroke 2012 (Epub ahead of print; DOI: 10.1161/STROKEAHA.112.655894)
Background
Hypercholesteremia increases the risk of ischemic stroke [1-5]. Lipid lowering treatment with statins reduces CV mortality by preventing myocardial infarction and ischemic stroke. This study examined the risk of hemorrhagic stroke in patients treated with statins, evaluated the effect of statins on total stroke and all-cause mortality, and determined whether hemorrhagic stroke was related to change in LDL-cholesterol. All available RCTs of statin therapy reporting hemorrhagic stroke rate were included in a meta-analysis.
Main results
- Statin treatment was not associated with increased incidence of intracerebral hemorrhage (ICH) (OR, 1.08; 95% CI, 0.88-1.32; P=0.47) (figure 1).
- There was no relationship between level of LDL cholesterol and effects of treatment on ICH risk.
- Total stroke was significantly reduced by statin treatment (OR, 0.84; 95% CI, 0.78-0.91, P< 0.0001)
- The rate of all-cause mortality was significantly lower in the statin-treated group (OR, 0.92; 95% CI, 0.87-0.96; P=0.0007)
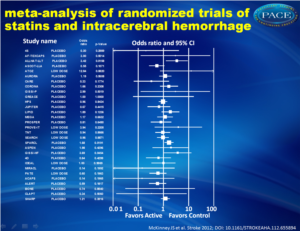 Figure 1.Forrest plot of random-effects meta-analysis of randomized trials of statins and intracerebral hemorrhage.Click on image to enlarge See left column to download as PowerPoint |
Conclusion
Statin therapy was not associated with a significant increased risk of ICH. The significant reductions in total stroke and all-cause mortality support the recommendations to prescribe statins in an unselected patient population.
References
1. Iso H, Jacobs DR Jr, et al. Serum cholesterol levels and six-year mortality from stroke in 350 977 men screened for the multiple risk factor intervention trial. N Engl J Med.1989;320:904 –910.2. Leppala JM, Virtamo J, et al. Different risk factors for different stroke subtypes: association of blood pressure, cholesterol, and antioxidants. Stroke. 1999;30:2535–2540.
3. Horenstein RB, Smith DE, Mosca L. Cholesterol predicts stroke mortality in the women’s pooling project. Stroke. 2002;33:1863–1868.
4. Zhang X, Patel A, et al. Cholesterol, coronary heart disease, and stroke in the Asia Pacific region. Int J Epidemiol. 2003;32:563–572.
5. Kurth T, Everett BM, et al. Lipid levels and the risk of ischemic stroke in women. Neurology. 2007;68:556 –562.
Abstract
Background and PurposeStatin therapy decreases the risk of ischemic stroke. An increased risk of intracerebral hemorrhage (ICH) has been observed in some studies. To investigate this issue, we performed a meta-analysis of randomized controlled trials using statins that reported ICH.
Methods
We performed a literature search of Medline, Web of Science, and The Cochrane Library through January 25, 2012, and identified additional randomized controlled trials by reviewing reference lists of retrieved studies and prior meta-analyses. All randomized controlled trials of statin therapy that reported ICH or hemorrhagic stroke were included. The primary outcome variable was ICH. Thirty-one randomized controlled trials were included. All analyses used random effects models and heterogeneity was not observed in any of the analyses.
Results
A total of 91 588 subjects were included in the active group and 91 215 in the control group. There was no significant difference in incidence of ICH observed in the active treatment group versus control (OR, 1.08; 95% CI, 0.88 –1.32; P=0.47). ICH risk was not related to the degree of low-density lipoprotein reduction or achieved low-density lipoprotein cholesterol. Total stroke (OR, 0.84; 95% CI, 0.78–0.91; P<0.0001) and all-cause mortality (OR, 0.92; CI, 0.87– 0.96; P=0.0007) were significantly reduced in the active therapy group. There was no evidence of publication bias.
Conclusions
Active statin therapy was not associated with significant increase in ICH in this meta-analysis of 31 randomized controlled trials of statin therapy. A significant reduction in all stroke and all-cause mortality was observed with statin therapy.
