Chronic kidney disease and coronary risk
This study assessed whether CKD should be considered as a chronic heart disease equivalent. Data from a population-based cohort were analyzed, comparing the incidence of heart attacks and death in patients with chronic kidney disease, diabetes, at least one previous heart attack, or a combination of these risk factors.
Risk of coronary events in people with chronic kidney disease compared with those with diabetes: a population-level cohort studyLiterature - Tonelli M et al, The Lancet, 19 June 2012
Tonelli M, Muntner P, Lloyd A, et al, for the Alberta Kidney Disease Network
The Lancet, Early Online Publication, 19 June 2012 doi:10.1016/S0140-6736(12)60572-
Background
Lipid-lowering treatment should be initiated in patients with coronary heart disease or an equivalent disorder [1]. A coronary heart disease risk equivalent is a characteristic leading to a 10-year risk of coronary death or myocardial infarction equivalent to the risk associated with previous myocardial infarction (risk generally >20%) [2]. Diabetes is classified as a coronary heart disease equivalent – people with diabetes have a very high risk of cardiovascular events [3] and should be eligible for lipid-lowering treatmentIt is unknown whether chronic kidney disease is also a coronary heart disease risk equivalent, especially chronic kidney disease including proteinuria. This study assessed whether CKD should be considered as a chronic heart disease equivalent. Data from a population-based cohort from 1.25 million people in Alberta, Canada were analyzed, comparing the incidence of heart attacks and death in patients with chronic kidney disease, diabetes, at least one previous heart attack, or a combination of these risk factors.
Main results
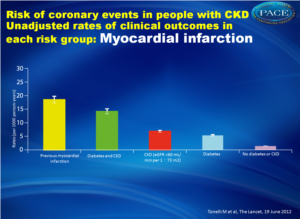
During a median follow-up of 4 years, 11,340 people were admitted to the hospital for MI.People with a previous MI were at higher risk for MI admission than people with either diabetes or CKD:
- MI history: 18.5 per 1000 person-years (CI 17.4–19.8)
- Diabetes: 5.4 per 1000 person-years (5.2–5.7)
- CKD: 6.9 per 1000 person-years (6.6–7.2)
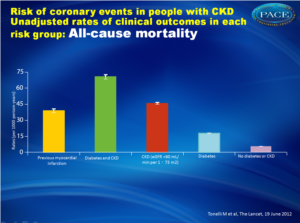
- Previous MI: 7.7%, RR 3.8 (CI 3.5-41)
- Diabetes and CKD: 6%, RR 2.7 (2.5-2.9)
- CKD: 2.8%, RR 1.4 (1.3-3.5)
- Diabetes: 2.4%, RR 2.0 (1.9-2.1)
- No diabetes or CKD: 0.5%, RR 1 (reference)
Conclusion
People with chronic kidney disease, diabetes, or both, tended to experience a comparable risk of heart attack to those who had previously had a heart attack, suggesting that kidney disease could prove to be a useful prognostic marker for coronary heart disease.
Editorial comment [4]
The results should be interpreted with caution. The study’s large scale is an advantage, a lack of information about individuals’ medication and other factors such as blood pressure means that the findings don’t necessarily provide clear-cut support for the classification of chronic kidney disease as a coronary heart disease risk equivalent. However, even if further analysis fails to support the classification of chronic kidney disease as a coronary heart disease risk equivalent, compelling reasons are provided to consider lipid-lowering therapy in patients with chronic kidney disease.
References
1. Third report of the National Cholesterol Education Program (NCEP) expert panel on detection, evaluation, and treatment of high blood cholesterol in adults (Adult Treatment Panel III) final report. Circulation 2002; 106: 3143–421.
2. Grundy SM. Diabetes and coronary risk equivalency: what does it mean? Diabetes Care 2006; 29: 457–60.
3. Haffner SM, Lehto S, Ronnemaa T, et al. Mortality from coronary heart disease in subjects with type 2 diabetes and in nondiabetic subjects with and without prior myocardial infarction. N Engl J Med 1998; 339: 229–34.
4. Polonsky TS, Bakris GL. Chronic kidney disease: a coronary heart disease equivalent? The Lancet, Early Online Publication, 19 June 2012 doi:10.1016/S0140-6736(12)60772-7
Abstract
Background:Diabetes is regarded as a coronary heart disease risk equivalent—ie, people with the disorder have a risk of coronary events similar to those with previous myocardial infarction. We assessed whether chronic kidney disease should be regarded as a coronary heart disease risk equivalent.measures of estimated glomerular filtration rate (eGFR) and proteinuria from Alberta, Canada. We used validated algorithms based on hospital admission and medical-claim data to classify participants with baseline history of myocardial infarction or diabetes and to ascertain which patients were admitted to hospital for myocardial infarction during follow-up (the primary outcome). For our primary analysis, we defined baseline chronic kidney disease as eGFR 15—59•9 mL/min per 1•73 m2 (stage 3 or 4 disease). We used Poisson regression to calculate unadjusted rates and relative rates of myocardial infarction during follow-up for five risk groups: people with previous myocardial infarction (with or without diabetes or chronic kidney disease), and (of those without previous myocardial infarction), four mutually exclusive groups defined by the presence or absence of diabetes and chronic kidney disease.
Findings:
During a median follow-up of 48 months (IQR 25—65), 11 340 of 1 268 029 participants (1%) were admitted to hospital with myocardial infarction. The unadjusted rate of myocardial infarction was highest in people with previous myocardial infarction (18•5 per 1000 person-years, 95% CI 17•4—19•8). In people without previous myocardial infarction, the rate of myocardial infarction was lower in those with diabetes (without chronic kidney disease) than in those with chronic kidney disease (without diabetes; 5•4 per 1000 person-years, 5•2—5•7, vs 6•9 per 1000 person-years, 6•6—7•2; p<0•0001). The rate of incident myocardial infarction in people with diabetes was substantially lower than for those with chronic kidney disease when defined by eGFR of less than 45 mL/min per 1•73 m2 and severely increased proteinuria (6•6 per 1000 person-years, 6•4—6•9 vs 12•4 per 1000 person-years, 9•7—15•9).
Interpretation:
our findings suggest that chronic kidney disease could be added to the list of criteria defining people at highest risk of future coronary events.