ARISTOTLE: effect of apixaban in relation to renal function
11/09/2012
The effect of apixaban, a novel oral anticoagulant, on the rate of stroke, death, and bleeding among patients with atrial fibrillation in relation to renal function.
Figure 1.Literature - Hohnloser SH et al, Eur Heart J 2012;Aug 29
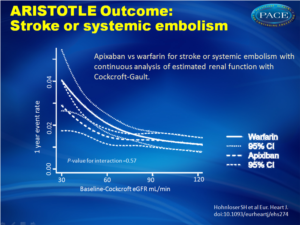 Apixaban vs warfarin for stroke or systemic embolism with continuous analysis of estimated renal function with Cockcroft-Gault Apixaban vs warfarin for stroke or systemic embolism with continuous analysis of estimated renal function with Cockcroft-Gault |
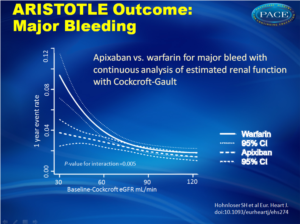 Figure 2Apixaban vs. warfarin for major bleed with continuous analysis of estimated renal function with Cockcroft-Gault. |
Conclusion
When compared with warfarin, apixaban treatment reduced the rate of stroke, death, and major bleeding, regardless of renal function. Apixaban seems to be an appealing option for individuals with impaired renal function, potentially leading to a substantial increase in the numbers of appropriately anticoagulated patients.
References
1. Go AS, Fang MC, Udaltsova N, et al. Impact of proteinuria and glomerular filtration rate on risk of thromboembolism in atrial fibrillation: the anticoagulation and risk factors in atrial fibrillation (ATRIA) study. Circulation 2009;119:1363–1369.2. Piccini JP, Hernandez AF, Zhao X, et al. Quality of care for atrial fibrillation among patients hospitalized for heart failure. J Am Coll Cardiol 2009;54:1280–1289.
3. Marinigh R, Lane DA, Lip GYH. Severe renal impairment and stroke prevention in atrial fibrillation. Implications for thromboprophylaxis and bleeding risk. J Am Coll Cardiol 2011;57:1339–1348.
4. Granger CB, Alexander JH, McMurray JJ, et al. Apixaban versus warfarin in patients with atrial fibrillation. N Engl J Med 2011;365:981–992.
5. Lopes RD, Alexander JH, Al-Khatib SM, et al. Apixaban for reduction in stroke and other thromboembolic events in atrial fibrillation (ARISTOTLE) trial: design and rationale. Am Heart J 2010;159:331–339.
6. Levey AS, Stevens LA, Schmid CH, et al. A new equation to estimate glomerular filtration rate. Ann Intern Med 2009;150:604–612.
7. Laterza OF, Price CP, Scott MG. Cystatin C: an improved estimator of glomerular filtration rate? Clin Chem 2002;48:699–707.
Abstract
AimsAtrial fibrillation (AF) is common among patients with impaired renal function. Apixaban, a novel oral anticoagulant with partial renal excretion, was compared with warfarin and reduced the rate stroke, death and bleeding in the ARISTOTLE trial. We evaluated these outcomes in relation to renal function.
Methods and results
Baseline glomerular filtration rate (GFR) was estimated using the Cockcroft–Gault and Chronic Kidney Disease Epidemiology Collaboration (CKD-EPI) equations as well as cystatin C measurements. According to baseline Cockcroft– Gault, there were 7518 patients (42%) with an estimated GFR (eGFR) of .80 mL/min, 7587 (42%) between .50 and 80 mL/min, and 3017 (15%) with an eGFR of ≤50 mL/min. The rate of cardiovascular events and bleeding was higher at impaired renal function (≤80 mL/min). Apixaban was more effective than warfarin in preventing stroke or systemic embolism and reducing mortality irrespective of renal function. These results were consistent, regardless of methods for GFR estimation. Apixaban was associated with less major bleeding events across all ranges of eGFRs. The relative risk reduction in major bleeding was greater in patients with an eGFR of ≤50 mL/min using Cockcroft– Gault {hazard ratio (HR) 0.50 [95% confidence interval (CI) 0.38–0.66], interaction P ¼ 0.005} or CKD-EPI equations [HR 0.48 (95% CI 0.37–0.64), interaction P ¼ 0.003].
Conclusion
In patients with AF, renal impairment was associated with increased risk of cardiovascular events and bleeding. When compared with warfarin, apixaban treatment reduced the rate of stroke, death, and major bleeding, regardless of renal function. Patients with impaired renal function seemed to have the greatest reduction in major bleeding with apixaban.
