Kidney function linked to thrombosis?
25/10/2012
The association of CKD with venous thrombosis was assessed in 5 general population cohorts.
Literature - Mahmoodi BK et al, Circulation. 2012;126(16):1964-71Mahmoodi BK, Gansevoort RT, Næss IA, et al.
Circulation. 2012;126(16):1964-71.
Background
Chronic kidney disease (CKD) affects 10% to 16% of the general adult population [1-4]. Associations of CKD with arterial thromboembolism and mortality are well known. However, the association of CKD with venous thromboembolism (VTE) is uncertain. In the present study, the association of CKD with venous thrombosis was assessed in 5 general population cohorts involving 95,514 participants.
Main results
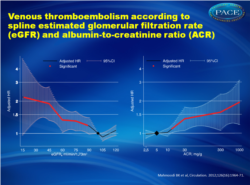
- The key CKD measures (ie, decreased estimated glomerular filtration rate (eGFR) and elevated albumin-to-creatinine ratio (ACR)) were both associated with an increased risk of VTE, even for values in the normal ranges.
- Individuals with an eGFR of 75 ml/min per 1.73 m2 had a 29% higher risk for VTE than those with an eGFR of 100 ml/min per 1.73 m2.
- This heightened risk worsened as eGFR levels fell, with a 31% increased risk for VTE among those with an eGFR of 60 ml/min per 1.73 m2, an 82% increased risk for those with an eGFR of 45 ml/min per 1.73 m2, and a 95% increased risk for those with an eGFR of 30 ml/min per 1.73 m2.
- Compared with individuals who had an ACR of 5.0 mg/g, those with an ACR of 30 mg/g were at a 34% higher risk for VTE, those with an ACR of 300 mg/g were at a 60% higher risk, and those with an ACR of 1000 mg/g at a 92% higher risk.
- There was no significant interaction between clinical categories of eGFR and ACR.
- Individuals diagnosed with chronic kidney disease (CKD; defined as eGFR <60 ml/min/1.73 m2 or albuminuria ≥30 mg/g) had a significant 54% higher risk for VTE than those without CKD.
Conclusion
Both eGFR and ACR are independently associated with increased risk of VTE in the general population, even in the non-CKD range of eGFR and the normal range of ACR.Future studies are warranted to assess whether CKD is also associated with recurrent VTE, which may have implications for the duration of anticoagulant treatment for first VTE.
Editorial comment [5]
“Patients with CKD should be carefully evaluated not only for abnormalities related to hypertension, athero- and arteriosclerosis, left ventricular hypertrophy, and arrhythmia, but also for abnormalities on the venous side of the vasculature. This provides more reason for close cooperation among cardiologists and nephrologists and an extension of the long list of cardiorenal syndromes.”
References
- Chadban SJ, Briganti EM, Kerr PG, et al. Prevalence of kidney damage in Australian adults: The AusDiab kidney study. J Am Soc Nephrol. 2003;14:S131–138.
- Coresh J, Selvin E, Stevens LA, et al. Prevalence of chronic kidney disease in the United States. JAMA. 2007;298:2038 –2047.
- Hallan SI, Coresh J, Astor BC, et al. International comparison of the relationship of chronic kidney disease prevalence and ESRD risk. J Am Soc Nephrol. 2006;17:2275–2284.
- Wen CP, Cheng TY, Tsai MK, et al. All-cause mortality attributable to chronic kidney disease: a prospective cohort study based on 462 293 adults in Taiwan. Lancet. 2008;371:2173–2182.
- Chertow GM, Mahaffey KW. Venous thromboembolism: yet another cardiovascular complication of chronic kidney disease? Circulation. 2012;126(16):1937-8.
Abstract
Background:Recent findings suggest that chronic kidney disease (CKD) may be associated with an increased risk of venous thromboembolism (VTE). Given the high prevalence of mild-to-moderate CKD in the general population, in depth analysis of this association is warranted.
Methods and results:
We pooled individual participant data from 5 community-based cohorts from Europe (second Nord-Trøndelag Health Study [HUNT2], Prevention of Renal and Vascular End-stage Disease [PREVEND], and the Tromsø study) and the United States (Atherosclerosis Risks in Communities [ARIC] and Cardiovascular Health Study [CHS]) to assess the association of estimated glomerular filtration rate (eGFR), albuminuria, and CKD with objectively verified VTE. To estimate adjusted hazard ratios for VTE, categorical and continuous spline models were fit by using Cox regression with shared-frailty or random-effect meta-analysis. A total of 1178 VTE events occurred over 599 453 person-years follow-up. Relative to eGFR 100 mL/min per 1.73 m(2), hazard ratios for VTE were 1.29 (95% confidence interval, 1.04-1.59) for eGFR 75, 1.31 (1.00-1.71) for eGFR 60, 1.82 (1.27-2.60) for eGFR 45, and 1.95 (1.26-3.01) for eGFR 30 mL/min per 1.73 m(2). In comparison with an albumin-to-creatinine ratio (ACR) of 5.0 mg/g, the hazard ratios for VTE were 1.34 (1.04-1.72) for ACR 30 mg/g, 1.60 (1.08-2.36) for ACR 300 mg/g, and 1.92 (1.19-3.09) for ACR 1000 mg/g. There was no interaction between clinical categories of eGFR and ACR (P=0.20). The adjusted hazard ratio for CKD, defined as eGFR <60 mL/min per 1.73 m(2) or albuminuria ≥30 mg/g, (versus no CKD) was 1.54 (95% confidence interval, 1.15-2.06). Associations were consistent in subgroups according to age, sex, and comorbidities, and for unprovoked versus provoked VTE, a
Conclusions:
Both eGFR and ACR are independently associated with increased risk of VTE in the general population, even across the normal eGFR and ACR ranges.