Mortality prediction based on BP trends
05/12/2012
J. Hypertension, Nov 2012. Study shows the importance of repeated blood pressure measurement in recognizing trends in systolic blood pressure and SBP value at the age of 90 for the prediction of mortality.
Blood pressure trends and mortality: the Leiden 85-plus Study.Literature - Poortvliet RK et al, J Hypertens. 2012 Nov 23
Poortvliet RK, de Ruijter W, de Craen AJ, et al.
J Hypertens. 2012 Nov 23. [Epub]
In elderly people, hypertension is a common condition [1,2]. The association between a single blood pressure measurement and mortality in very old people is unclear; data are often conflicting. The association between SBP trends and mortality was studied in a cohort of 90-years old from the Leiden 85-plus Study. Independent contributions of both current SBP value at age 90 and the trend in preceding SBP measurements to the prediction of mortality at age 90 were evaluated.
2. Aguado A, Lopez F, Miravet S, et al. Hypertension in the very old; prevalence, awareness, treatment and control: a cross-sectional population-based study in a Spanish municipality. BMC Geriatr 2009; 9:16.
Objective:
To evaluate the independent contributions of both the trend in SBP and the SBP value at age 90 to the prediction of mortality in nonagenarians.
Methods:
The trend in SBP between 85 and 90 years and SBP at age 90 years were assessed in a population-based sample of 271 participants (74 men and 197 women) aged 90 years of the Leiden 85-plus Study, an observational population-based prospective follow-up study (started 1997). Primary endpoint, followed up over 5 years (median 3.6 years), was all-cause mortality.
Results:
A decreasing trend in SBP between 85 and 90 years (decline ≥2.9 mmHg/year) was associated with increased mortality compared to an average SBP trend (hazard ratio 1.45, 95% confidence interval 1.02-2.06), independent of SBP at age 90. The effect was stronger in institutionalized participants compared to those living independently [hazard ratio 1.87 (1.10-3.19) and hazard ratio 1.30 (0.81-2.09)]. After analysis with a fully adjusted model, the estimate approached unity [hazard ratio 1.08 (0.60-1.86)]. Overall, 90-year-old participants with SBP of 150 mmHg or less had a 1.62 times increased mortality risk compared to those with SBP more than 150 mmHg (1.21-2.20), independent of the SBP trend in preceding years. This applied to those with and without antihypertensive drugs and those with and without history of cardiovascular disease or noncardiovascular disease. In the fully adjusted model, the estimate was 1.47 (0.90-2.40). Conclusion: In very old age, both decreasing trend in SBP over the previous 5 years and the current SBP value independently contribute to prediction of all-cause mortality. Therefore, in individual patients, all available preceding SBP measurements should be taken into account.
J Hypertens. 2012 Nov 23. [Epub]
Background
In elderly people, hypertension is a common condition [1,2]. The association between a single blood pressure measurement and mortality in very old people is unclear; data are often conflicting. The association between SBP trends and mortality was studied in a cohort of 90-years old from the Leiden 85-plus Study. Independent contributions of both current SBP value at age 90 and the trend in preceding SBP measurements to the prediction of mortality at age 90 were evaluated.
Main results
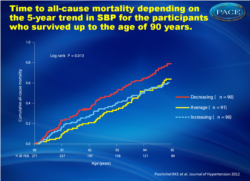
- A decreasing 5-year trend in SBP (≥2.9 mmHg/year) was associated with an increased cumulative all-cause mortality compared to an increasing or average 5-year trend (fig. 1).
- Participants with a decreasing 5-year trend in SBP had a 1.5-fold increased all-cause mortality risk compared to those with an average SBP trend (HR 1.51, 95% CI 1.07-2.15)
- Adjusted for SBP at age 90, participants with a decreasing 5-year trend in SBP had an increased all-cause mortality risk compared to those with an average SBP trend (HR 1.45, 95% CI 1.02-2.06). This association was stronger in institutionalized individuals i.e. the most frail elderly subjects.
- Participants with a low SBP at age 90 had an increased all-cause mortality risk compared to those with a high SBP (HR 1.57, 95% CI 1.18–2.09).
- Adjusted for SBP trends, participants with a low SBP at age 90 had a 1.6-fold increased all-cause mortality risk compared to those with a high SBP (HR 1.62, 95% CI 1.21–2.20).
- After full adjustment including all baseline characteristics and SBP trends, participants with a low SBP at age 90 had a 1.5-fold increased all-cause mortality risk compared to those with a high SBP at age 90 years (HR 1.47, 95% CI 0.90–2.40).
Conclusion
In very old age, all available preceding SBP measurements contribute to a more accurate prediction of mortality and should be taken into account. In addition, repeated blood pressure measurement may contribute to identification of older people at risk.References
1. de Craen AJ, Gussekloo J, Teng YK, et al. Prevalence of five common clinical abnormalities in very elderly people: population based cross sectional study. BMJ 2003; 327:131–132.2. Aguado A, Lopez F, Miravet S, et al. Hypertension in the very old; prevalence, awareness, treatment and control: a cross-sectional population-based study in a Spanish municipality. BMC Geriatr 2009; 9:16.
Abstract
Objective:To evaluate the independent contributions of both the trend in SBP and the SBP value at age 90 to the prediction of mortality in nonagenarians.
Methods:
The trend in SBP between 85 and 90 years and SBP at age 90 years were assessed in a population-based sample of 271 participants (74 men and 197 women) aged 90 years of the Leiden 85-plus Study, an observational population-based prospective follow-up study (started 1997). Primary endpoint, followed up over 5 years (median 3.6 years), was all-cause mortality.
Results:
A decreasing trend in SBP between 85 and 90 years (decline ≥2.9 mmHg/year) was associated with increased mortality compared to an average SBP trend (hazard ratio 1.45, 95% confidence interval 1.02-2.06), independent of SBP at age 90. The effect was stronger in institutionalized participants compared to those living independently [hazard ratio 1.87 (1.10-3.19) and hazard ratio 1.30 (0.81-2.09)]. After analysis with a fully adjusted model, the estimate approached unity [hazard ratio 1.08 (0.60-1.86)]. Overall, 90-year-old participants with SBP of 150 mmHg or less had a 1.62 times increased mortality risk compared to those with SBP more than 150 mmHg (1.21-2.20), independent of the SBP trend in preceding years. This applied to those with and without antihypertensive drugs and those with and without history of cardiovascular disease or noncardiovascular disease. In the fully adjusted model, the estimate was 1.47 (0.90-2.40). Conclusion: In very old age, both decreasing trend in SBP over the previous 5 years and the current SBP value independently contribute to prediction of all-cause mortality. Therefore, in individual patients, all available preceding SBP measurements should be taken into account.