High risk people with CVD in Chinese rural areas characterised
01/02/2013
In the context of primary care, a holistic strategy focused on population with high risk CVD is recommended. Very few patients took any drugs, and less still took highly effective drugs to prevent CVD.
AbstractLiterature - Wei X, Zou G, Yin J, et al. - PLoS One. 2013;8(1):e54169. doi: 10.1371/journal.pone.0054169.
Characteristics of high risk people with cardiovascular disease in chinese rural areas: clinical indictors, disease patterns and drug treatment.
Wei X, Zou G, Yin J, et al.
PLoS One. 2013;8(1):e54169. doi: 10.1371/journal.pone.0054169.
Background
Cardiovascular disease (CVD) is the leading cause of death in China, accounting for 38% of total mortality. In 2006, there were approximately 160 million Chinese people with hypertension, 160 million with hyperlipidaemia, 20 million with diabetes and 200 million who were overweight [1]. Chinese people has a higher risk of haemorrhagic stroke compared with the Western population [2]. Treatment with two antihypertensive drugs simultaneously will reduce the risk of stroke by 63% and ischaemic disease by 46% [3], while statins will reduce the risk by 60% and 17% respectively [4]. The combined effects of three antihypertensive drugs, plus a statin and aspirin would reduce by more than 88% ischaemic heart disease events and by 80% stroke events [5].Current CVD prevention is based on diagnosis and treatment of specific disease. However, little is known for high risk people with CVD at the community level. In rural China, health records of all residents were established after the recent health reforms.
Main results
- Residents who had a CVD risk of ≥ 20% were selected for a face-to-face questionnaire survey regarding their diagnosed disease and drug treatment.
- Of the identified individuals with a high risk of CVD (n = 453) had an average age of 53 years; 62% were male, smoking rate was 50% and the average systolic blood pressure was 161 mmHg.
- 19% took drug regularly and 32% either stopped treatment or missed drugs. The most often used drugs were calcium channel blockers (20%). Only 2% used aspirins and 0.8% used statins.
Conclusion
The majority of the high risk population in our setting of rural China had already been diagnosed with a CVD related disease, but very few took any drugs, and less still took highly effective drugs to prevent CVD. A holistic strategy focused on population with high risk CVD and based on the current China public health reform is suggested in the context of primary care.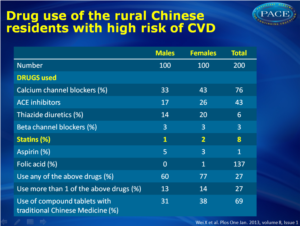 Table 1.Drug use of the 200 rural residents with high CVD risk, who were treated in a rural primary care setting in Zhejiang China |
References
1. National Centre for Cardiovascular Disease. Report on the cardiovascular disease in China 2007. Beijing: Encyclopedia of China Publishing House.2. WHO. Global status report on on noncommunicable diseases. 2010: 1–176.
3. Law MR, Wald NJ, Morris JK, Jordan RE. Value of low dose combination treatment with blood pressure lowering drugs: analysis of 354 randomised trials. BMJ 2003;326: 1427.
4. Law MR, Wald NJ, Rudnicka AR. Quantifying effect of statins on low density lipoprotein cholesterol, ischaemic heart disease, and stroke: systematic review and meta-analysis. BMJ 2003; 326: 1423.
5. Wald NJ, Law MR. A strategy to reduce cardiovascular disease by more than 80%. BMJ 2003;326: 1419.Background:
Current cardiovascular disease (CVD) prevention is based on diagnosis and treatment of specific disease. Little is known for high risk people with CVD at the community level. In rural China, health records of all residents were established after the recent health reforms.
Objectives:
This study aims to describe the characters of the rural population with high CVD risk regarding their clinical indicators, disease patterns, drug treatment and adherence.
Methods and results:
17042 (87%) of all the 19500 rural residents in the two townships had valid health records in 2009. We employed a validated tool, the Asian Equation, to screen 8182 (48%) resident health records of those aged between 40-75 years in 2010. Those who were identified with a CVD risk of 20% or higher were selected for a face-to-face questionnaire survey regarding their diagnosed disease and drug treatment. 453 individuals were identified as high risk of CVD, with an average age of 53 years, 62% males, 50% smoking rate and average systolic blood pressure of 161 mmHg. 386 (85%) participated in the survey, while 294 (76%) were diagnosed with and 88 (23%) were suspects of CVD, hypertension, diabetes or hyperlipidaemia. 75 (19%) took drug regularly and 125 (32%) either stopped treatment or missed drugs. The most often used drugs were calcium channel blockers (20%). Only 2% used aspirins and 0.8% used statins. The median costs of drugs were 17 RMB (USD2.66) per month.
Conclusions:
The majority of the high risk population in our setting of rural China had already been diagnosed with a CVD related disease, but very few took any drugs, and less still took highly effective drugs to prevent CVD. A holistic strategy focused on population with high risk CVD and based on the current China public health reform is suggested in the context of primary
