BMI affects CV outcomes in hypertensive patients
13/03/2013
Non-obese patients are better protected by calcium-channel blocker-based therapy, whereas obese patients benefit equally well from diuretic-based therapy.
AbstractLiterature - Weber MA, Jamerson K, Bakris GL, et al. - Lancet. 2013 Feb 16;381(9866):537-45. doi: 10.1016/S0140-6736(12)61343-9.
Effects of body size and hypertension treatments on cardiovascular event rates: subanalysis of the ACCOMPLISH randomised controlled trial.
Weber MA, Jamerson K, Bakris GL, et al.
Lancet. 2013 Feb 16;381(9866):537-45. doi: 10.1016/S0140-6736(12)61343-9.
Background
Obesity is commonly associated with a high incidence of cardiovascular events. Interestingly enough, individuals with normal body weight with established cardiovascular disease (CVD), appear to suffer from higher incidence rates [1-3]. Similarly, lean hypertensive individuals have a higher incidence of adverse cardiovascular outcomes than their obese counterparts [4-6]. A clinical trial of hypertensive treatments showed increased CV rates in lean, as opposed to overweight individuals [7]. Unfortunately it could not be concluded from this study whether this obesity paradox was due to innate clinical characteristics, or an effect of the study drugs, because all patients received active treatment.The randomised, double-blind, multicentre Avoiding Cardiovascular Events through Combination Therapy in Patients Living with Systolic Hypertension (ACCOMPLISH) trial is an opportunity to study effect of body weight and different treatment regimens in high risk hypertensive patients, as it compares CV outcomes in diuretic (benazepril + hydrochlorothiazide) vs non-diuretic (benazepril + amlodipine) drug regimens. This prespecified analysis provides insight into how treatment affects CV event rates in hypertensive patients, categorized by BMI [8].
Main results
- Cardiovascular event rate is significantly lower in obese (BMI>30) hypertensive patients, as compared to normal weight (BMI: 20-25) hypertensive patients (HR: 0.74, 95%CI: 0.59-0.92, P=0.0066)
- Different treatment regimens were equally effective in reducing endpoint CV event rates in obese patients. Endpoint event rate was lower in overweight patients (BMI: 25-30) treated with benazepril and amlodipine. This difference was even larger in normal weight patients.
Conclusion
Type of treatment is a determinant of the relation between body mass and CV outcome. Both treatment regimens were effective in obese patients. However, lean patients are better protected against CV events when given a treatment that includes a calcium-channel blocker, as opposed to thiazide-based therapy. The authors discuss that hypertension in obese and lean people is likely mediated by different underlying pathophysiology, which could explain the different effects of treatment seen in different weight groups.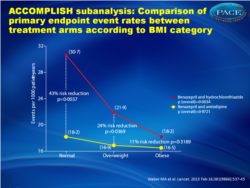 Differential effect of BMI on CV event rates depending on treatment regimen in hypertensive patients Differential effect of BMI on CV event rates depending on treatment regimen in hypertensive patients |
References
1.Curtis JP, Selter JG, Wang Y, et al. The obesity paradox: body mass index and outcomes in patients with heart failure. Arch Intern Med 2005; 165: 55–61.2. Gruberg L, Weissman NJ, Waksman R, et al. The impact of obesity on the short-term and long-term outcomes after percutaneous coronary intervention: the obesity paradox? J Am Coll Cardiol 2002; 39: 578–84.
3. Kang X, Shaw LJ, Hayes SW, et al. Impact of body mass index on cardiac mortality in patients with known or suspected coronary artery disease undergoing myocardial perfusion single-photon emission computed tomography. J Am Coll Cardiol 2006; 47: 1418–26.
4. Barrett-Connor E, Khaw K. Is hypertension more benign when associated with obesity? Circulation 1985; 72: 53–60.
5. Goldbourt U, Holtzman E, Cohen-Mandelzweig L, Neufeld HN. Enhanced risk of coronary heart disease mortality in lean hypertensive men. Hypertension 1987; 10: 22–28.
6.Carman WJ, Barrett-Connor E, Sowers M, Khaw K. Hypertension/risk factors: higher risk of cardiovascular mortality among lean hypertensive individuals in Tecumesh, Michigan. Circulation 1994; 89: 703–11.
7.Uretsky S, Messerli FH, Bangalore S, et al. Obesity paradox in patients with hypertension and coronary artery disease. Am J Med 2007; 120: 863–70.
8.Jamerson K, Weber MA, Bakris GL, et al. Benazepril plus amlodipine or hydrochlorothiazide for hypertension in high-riskpatients. N Engl J Med 2008; 359: 2417–28.BACKGROUND:
In previous clinical trials in high-risk hypertensive patients, paradoxically higher cardiovascular event rates have been reported in patients of normal weight compared with obese individuals. As a prespecified analysis of the Avoiding Cardiovascular Events through Combination Therapy in Patients Living with Systolic Hypertension (ACCOMPLISH) trial, we aimed to investigate whether the type of hypertension treatment affects patients' cardiovascular outcomes according to their body size.
METHODS:
On the basis of body-mass index (BMI), we divided the full ACCOMPLISH cohort into obese (BMI ≥30, n=5709), overweight (≥25 to <30, n=4157), or normal weight (<25, n=1616) categories. The ACCOMPLISH cohort had already been randomised to treatment with single-pill combinations of either benazepril and hydrochlorothiazide or benazepril and amlodipine. We compared event rates (adjusted for age, sex, diabetes, previous cardiovascular events, stroke, or chronic kidney disease) for the primary endpoint of cardiovascular death or non-fatal myocardial infarction or stroke. The analysis was by intention to treat. This trial is registered with ClinicalTrials.gov, number NCT00170950.
FINDINGS:
In patients allocated benazepril and hydrochlorothiazide, the primary endpoint (per 1000 patient-years) was 30•7 in normal weight, 21•9 in overweight, and 18•2 in obese patients (overall p=0•0034). However, in those allocated benazepril and amlodipine, the primary endpoint did not differ between the three BMI groups (18•2, 16•9, and 16•5, respectively; overall p=0•9721). In obese individuals, primary event rates were similar with both benazepril and hydrochlorothiazide and benazepril and amlodipine, but rates were significantly lower with benazepril and amlodipine in overweight patients (hazard ratio 0•76, 95% CI 0•59-0•94; p=0•0369) and those of normal weight (0•57, 0•39-0•84; p=0•0037).
INTERPRETATION:
Hypertension in normal weight and obese patients might be mediated by different mechanisms. Thiazide-based treatment gives less cardiovascular protection in normal weight than obese patients, but amlodipine-based therapy is equally effective across BMI subgroups and thus offers superior cardiovascular protection in non-obese hypertension.
