PCSK9 inhibitors reduce all-cause mortality but increase neurocognitive adverse events
This meta-analysis of RCTs compared the impact of PCSK9 inhibition alone, ezetimibe alone or the combination of these agents on lipid levels and clinical outcomes.
The impact of proprotein convertase subtilisinkexin type 9 serine protease inhibitors on lipid levels and outcomes in patients with primary hypercholesterolemia: a network meta-analysisLiterature - Lipinski MJ et al. Eur Heart J 2016
Lipinski MJ, Benedetto U, Escarcega RO, et al.
Eur Heart J 2016;37:536–545
Background
Lipid lowering therapy with statins is widely used for the primary and secondary prevention of major adverse cardiovascular (CV) and cerebrovascular events, particularly in patients at higher risk [1]. However, for some other lipid lowering agents such as niacin and the CETP inhibitor torcetrapib, data documented a lack of benefit, or even harm regarding clinical outcomes, despite significant reductions in LDL-c and increases in HDL-c [2,3]. Ezetimibe and PCSK9 inhibitors, however, have been associated with further LDL reduction and improved CV outcomes [4-6].In this network meta-analysis of 17 randomised controlled trials including 13,083 patients with primary hypercholesterolaemia, the impact of PCSK9 inhibitors alone, ezetimibe alone, or the combination of PCSK9 inhibitors and ezetimibe, on lipid levels and outcomes was assessed.
Main results
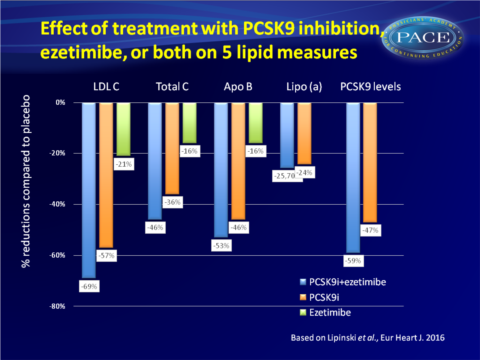
• Compared with placebo, tPCSK9 inhibition plus ezetimibe resulted in reduction of: LDL-c: 69%. total cholesterol: 46%, apolipoprotein B: 53%, lipoprotein(a): 25.7%, PCSK9: 59%.• Compared to placebo, PCSK9 inhibition alone led to: 57% lower LDL-c, 36% lower total cholesterol, 46% lower apolipoprotein B, 24.3% lower lipoprotein(a), 47% lower PCSK9 levels
• Compared to placebo, ezetimibe alone led to LDL-c: 21% reduction, total cholesterol: 16% reduction, apolipoprotein B: 16% reduction, no significant reduction of lipoprotein(a) and no impact on PCSK9 levels
• Relative to ezetimibe, PCSK9 inhibition alone reduced LDL-c by 36.1% (P < 0.001).
• In studies with high baseline statin use, PCSK9 inhibition led to a 57.8% decrease in LDL compared with placebo, and a 33.8% decrease in LDL compared with ezetimibe • In studies with low baseline statin use, PCSK9 inhibition led to a 53.8% decrease in LDL compared with placebo, and a 36.7% decrease in LDL compared with ezetimibe • Compared with placebo, PCSK9 inhibition :
- reduced the incidence of all-cause mortality (OR: 0.43, 95% CI: 0.22 – 0.82, P = 0.01)
- showed a trend toward reduced CV death (OR: 0.50, 95% CI: 0.22–1.13, P = 0.10)
- showed a trend toward reduced CV events (OR: 0.67, 95% CI: 0.43–1.04, P = 0.07)
- was associated with an increased incidence of neurocognitive adverse events (OR: 2.34, 95% CI: 1.11 –4.93, P = 0.02)
Conclusion
In patients with primary hypercholesterolemia, PCSK9 inhibition were associated with a significant improvement of lipid profiles, as well as with a reduction in all-cause mortality compared with placebo and ezetimibe. However, there was a higher rate of neurocognitive adverse events. PCSK9 inhibitors may serve as an alternative for patients with statin intolerance and for patients who do not respond to conventional lipid lowering therapy.Find this article online at Eur Heart J
References
1. Mega JL, Stitziel NO, Smith JG, et al. Genetic risk, coronary heart disease events, and the clinical benefit of statin therapy: an analysis of primary and secondary prevention trials. Lancet 2015; doi: 10.1016/S0140-6736(14)61730-X
2. Barter PJ, Caulfield M, Eriksson M, et al. Effects of torcetrapib in patients at high risk for coronary events. N Engl J Med 2007;357:2109–2122
3. AIM-HIGH Investigators, Boden WE, Probstfield JL, Anderson T, et al. Niacin in patients with low HDL cholesterol levels receiving intensive statin therapy. N Engl J Med 2011;365:2255–2267
4. Cannon CP, Blazing MA, Giugliano RP, et al. Ezetimibe added to statin therapy after acute coronary syndromes. N Engl J Med 2015, doi: 10.1056/NEJMoa1410489
5. Cohen JC, Boerwinkle E, Mosley TH Jr, et al. Sequence variations in PCSK9, low LDL, and protection against coronary heart disease. N Engl J Med 2006;354:1264–1272
6. Kotowski IK, Pertsemlidis A, Luke A, et al. A spectrum of PCSK9 alleles contributes to plasma levels of low-density lipoprotein cholesterol. Am J Hum Genet 2006;78:410–422
