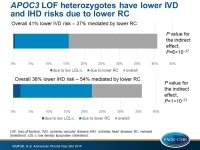
Remnant cholesterol determines CV risk in APOC3 LOF heterozygotes
The lower ischemic vascular risk in APOC3 loss-of-function heterozygotes compared with non-carriers is largely due to lower levels of remnant cholesterol, and not LDL-c, in these patients.
APOC3 Loss-of-Function Mutations, Remnant Cholesterol, Low-Density Lipoprotein Cholesterol, and Cardiovascular Risk: Mediation and Meta-Analyses of 137 895 IndividualsLiterature - Wulff AB, Nordestgaard BG and Tybjærg-Hansen A. - Arterioscler Thromb Vasc Biol 2018;38: published online ahead of
Background
//APOC3// loss-of-function (LOF) mutations have been associated with a lower risk of ischemic vascular disease (IVD), as well as with lower triglyceride, apolipoprotein CIII (ApoC3), and very LDL-c levels [1-4].
This study evaluated whether the low IVD risk in APOC3 LOF heterozygotes can be explained by the low plasma remnant cholesterol and low LDL-c levels. For this purpose, the levels of remnant cholesterol and LDL-c were determined in APOC3 LOF heterozygotes versus non-carriers, by means of a meta-analysis of 8 study cohorts including 137,895 individuals.
Moreover, LDL-c levels of APOC3 LOF heterozygotes were compared with those of non-carriers in 75,725 individuals in the two prospective Danish general population cohorts (Copenhagen City Heart Study and Copenhagen General Population Study), and it was assessed whether lipid-lowering therapy masked the associations of LDL cholesterol with IVD. Moreover, the fraction of the observed lower IVD and ischemic heart disease (IHD) risk associated with APOC3 LOF mutations was calculated using mediation analysis by low remnant cholesterol and low LDL-c.
Main results
- In the meta-analysis, APOC3 LOF heterozygotes had 43% (95%CI: 40%–47%) lower levels of remnant cholesterol compared with non-carriers in both a fixed and in a random effects model (no heterogeneity between studies (I2=0%; P=0.92)). APOC3 LOF heterozygotes had 4% (95%CI: 1%–6%) lower levels of LDL-c compared with non-carriers in a fixed effects model and 5% (95%CI: 1%–8%) lower levels of LDL-c in a random effects model.
- In the general population, remnant cholesterol was 44% (0.3 mmol/L) lower (P=1×10−51), and LDL-c was 3% (0.1 mmol/L) lower (P=0.06) in APO3 LOF heterozygotes versus non-carriers overall, regardless of lipid-lowering therapy.
- After correcting for lipid-lowering therapy, LOF heterozygotes in the general population had 43% (0.3 mmol/L) lower levels of remnant cholesterol (P=5×10−49) and 4% (0.1 mmol/L) lower levels of LDL-c (P=0.008) compared with non-carriers.
- When excluding participants on lipid-lowering therapy at the time of lipid assessment, remnant cholesterol was 44% (0.3 mmol/L) lower (P=2×10−49), and LDL-c was 3% (0.1 mmol/L) lower (P=0.02) in LOF heterozygotes compared with non-carriers.
- //APOC3// LOF heterozygotes showed significant median reductions of 47% (0.7 mmol/L) in triglycerides, 10% (0.4 mmol/L) in non-HDL-c and 13% (14 mg/dL) in apoB, as compared with noncarriers, and an increase of HDL-c of 33% (0.5 mmol/L).
- The mediation analysis showed that the lower levels of remnant cholesterol in LOF heterozygotes versus non-carriers mediated 37% of the lower IVD risk (P value for the indirect effect, P=6×10−37) and 54% of the lower IHD risk (P value for the indirect effect, P=1×10−37), whereas the 4% lower levels of LDL-c mediated only 1% and 2% of the lower risks.
Conclusion
The lower IVD risk in APOC3 LOF heterozygotes compared with non-carriers is largely due to the significantly lower levels of remnant cholesterol and not due to lower levels of LDL-c, and this observation was not affected by lipid-lowering therapy. These findings might be importantmay point at APOC3 and remnant cholesterol as therapeutic targets for CV prevention.
References
1. Jørgensen AB, Frikke-Schmidt R, Nordestgaard BG, et al. Loss-of-function mutations in APOC3 and risk of ischemic vascular disease. N Engl J Med. 2014;371:32–41.
2. Crosby J, Peloso GM, Auer PL, et al. Loss-of-function mutations in APOC3, triglycerides, and coronary disease. N Engl J Med. 2014;371:22–31.
3. Gaudet D, Alexander VJ, Baker BF, et al. Antisense inhibition of apolipoprotein C-III in patients with hypertriglyceridemia. N Engl J Med. 2015;373:438–447.
4. Gaudet D, Brisson D, Tremblay K, et al. Targeting APOC3 in the familial chylomicronemia syndrome. N Engl J Med. 2014;371:2200–2206.