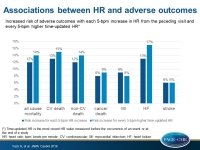
Increased resting heart rate and changes therein over time associated with adverse outcomes
In a community-based cohort, higher resting heart rate and increased changes in resting heart rate over time were associated with mortality, incident heart failure, myocardial infarction, and stroke.
Association of Resting Heart Rate and Temporal Changes in Heart Rate With Outcomes in Participants of the Atherosclerosis Risk in Communities StudyLiterature - Vazir A, Claggett B, Cheng S, et al. - JAMA Cardiol 2018; published online ahead of print
Background
Time-updated heart rate (HR) is the most recent HR value measured before the occurrence of an event or at the end of a study. ΔHR is the change in HR over time. Both measures have been associated with adverse cardiovascular (CV) outcomes in patients with heart failure (HF). More specifically; an increase in HR was associated with adverse outcomes and a decrease in HR was associated with better outcomes [1,2].
This analysis of the Atherosclerosis Risk in Communities (ARIC) study [3,4] evaluated whether time-updated HR and ΔHR are also associated with outcomes in a community-based cohort including 15,680 participants.
HR was recorded at baseline and during 3 follow-up visits from 1987 to 1998. The median interval between visits was 3.0 years (IQR: 2.9-4.0), and the follow-up duration was 28 years. Adjustments were made for established baseline and time-updated risk factors and treatments. The main outcome measures were all-cause mortality, incident HF, incident myocardial infarction (MI), stroke, as well as CV and non-CV death.
Main results
- Each 5-bpm increase in HR from the preceding visit (ΔHR) was significantly associated with a 12% (95%CI: 10%-15%; P<0.001) higher risk of all-cause mortality, a 13% (95%CI: 9%-16%: P<0.001) higher risk of incident HF, a 9% (95%CI: 4%-13%; P<0.001) higher risk of MI, a 6% (95%CI: 1%-11%; P=0.02) higher risk of stroke, a 13% (95%CI: 8%-17%; P<0.001) higher risk of CV death, a 12% (95% CI: 10%-15%; P<0.001) higher risk of non-CV death, and a 8% (95%CI: 3%-13%; P=0.001) higher risk of cancer death.
- Every 5-bpm higher time-updated HR was significantly associated with a 14% (95%CI: 12%-17%; P<0.001) higher risk of all-cause mortality, a 17% (95%CI: 14%-20%; P<0.001) higher risk of HF, an 8% (95%CI: 4%-12%; P<0.001) higher risk of MI, a 6% (95%CI: 1%-10%; P=0.01) higher risk of stroke, a 15% (95%CI: 11%-20%; P<0.001) higher risk of CV death, a 14% (95%CI: 11%-17%; P<0.001) higher risk of non-CV death, and a 9% (95%CI: 5%-14%; P<0.001) higher risk of cancer death.
- A lower time-updated HR was associated with a lower number of events. For example, time-updated HR values of 50-60 bpm were associated with a lower risk of all-cause mortality and a lower risk of incident HF compared with a time-updated HR of 60 bpm.
- Use of β-blockers at any time neutralized the associations between HR or ΔHR and all-cause mortality.
Conclusion
In a community-based cohort, increased time-updated HR and ΔHR were associated with mortality and non-fatal outcomes of incident HF, MI, and stroke. These results support the importance of measuring HR in every-day clinical practice, to identify individuals who might be at greater risk of adverse outcomes.
References
1. Paul L, Hastie CE, LiWS, et al. Resting heart rate pattern during follow-up and mortality in hypertensive patients. Hypertension. 2010;55(2):567-574.
2. Vazir A, Claggett B, Jhund P, et al. Prognostic importance of temporal changes in resting heart rate in heart failure patients: an analysis of the CHARM program. Eur Heart J. 2015;36(11):669-675.
3. The ARIC investigators. The Atherosclerosis Risk in Communities (ARIC) study: design and objectives. Am J Epidemiol. 1989;129(4):687-702.
4. Cheng S, Claggett B, Correia AW, et al. Temporal trends in the population attributable risk for cardiovascular disease: the Atherosclerosis Risk in Communities study. Circulation. 2014;130(10):820-828.