Intensive BP lowering also seems beneficial in adults with diabetes, irrespective of baseline BP
An analysis of the ADVANCE study shows that the treatment effect of perindopril-indapamide in patients with diabetes is independent of SBP, DBP or 10-year ASCVD risk at baseline.
Effects of Blood Pressure Lowering on Clinical Outcomes According to Baseline Blood Pressure and Cardiovascular Risk in Patients With Type 2 Diabetes Mellitus.Literature - Rahman F, McEvoy JW, Ohkuma T et al; ADVANCE Collaborative Group. - Hypertension. 2019 doi: 10.1161/HYPERTENSIONAHA.118.12414
Introduction and methods
Uncertainty surrounds the blood pressure (BP) threshold for initiation of antihypertensive therapy in patients with diabetes mellitus [1-3]. This complicates care of these patients, in light of their risk of future CV events that is associated with having diabetes.
Several recent studies in adults without diabetes provided support for BP targets that are lower than previously advised, for instance SPRINT [4] and HOPE-3 [5]. However, no participants in SPRINT and only 6% in HOPE-3 had diabetes. Trials that did study BP lowering in patients with diabetes show inconsistent results. The UKPDS data supported intensive BP reduction in adults with diabetes, but it is important to realize that the study started >25 years ago and the initial and achieved BPs were higher than what would be considered clinically safe today [6]. The more contemporary ACCORD trial did not show a CV outcome benefit of lowering BP to<120 mmHg as compared with <140 mmHg [7]. Recommended BP goals for diabetes patients in international guidelines vary [1-3].
ADVANCE provided additional support for intensive BP treatments among patients with diabetes [8]. This trial randomized participants to intensive therapy with a fixed combination of perindopril-indapamide or to placebo. The active arm showed an average reduction of BP of 5.6/2.2 mmHg, which was associated with 9% reduction in major macrovascular or microvascular events, and a 18% lower CV mortality [8].
This analysis (n=10.948) set out to examine whether the effects of intensification of BP therapy among people with diabetes in the ADVANCE trial, differed per SBP, DBP or estimated CV risk at baseline. The current analysis considered the composite outcome of major macrovascular and microvascular events and all-cause mortality as twin primary efficacy outcomes. Participants were categorized based on baseline SBP: <120, 120-129, 130-139, 140-149, 150-159 and ≥160 mmHg.
Main results
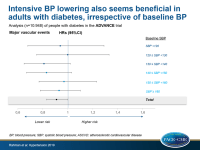
- Mean on-treatment BP was lower in the intervention arm than in the placebo-arm, which was consistent across all categories of 10-year ASCVD risk or baseline SBP.
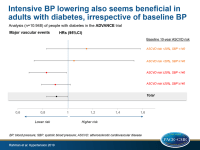
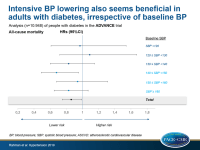
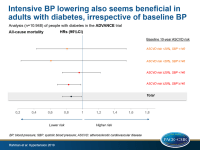
- Over a mean follow-up of 4.3 years, treatment with perindopril-indapamide was associated with a lower rate of major vascular events (HR: 0.91, 95%CI: 0.83-0.997) and all-cause mortality (HR: 0.86, 95%CI: 0.75-0.99). There was no evidence of heterogeneity in the treatment effect across SBP subgroups (major vascular events: P=0.83, all-cause mortality: P=0.36).
- Nor was heterogeneity of treatment effect seen when subgroups were defined by baseline DBP levels or by a combination of SBP and DBP).
- No evidence of heterogeneity was seen in treatment effect when subgroups were defined based on ASCVD risk.
- No statistically significant heterogeneity was seen in the rate of adverse events leading to permanent discontinuation of study drug when subgroups based on baseline SBP, DBP or 1-year ASCVD risk were considered.
Conclusion
This analysis of the ADVANCE trial shows that more intense antihypertensive treatment with a fixed combination of perindopril-indapamide lowered the rate of all-cause mortality and major vascular events in patients with diabetes. This treatment effect was independent by baseline BP or 10-year ASCVD risk. Moreover, the likelihood of common adverse side effects leading to permanent drug discontinuation, was not affected by baseline SBP <140 vs. ≥140 mmHg. This analysis supports more intensive BP-lowering treatment in patients with diabetes, regardless of BP and 10-year ASCVD risk at baseline. Nevertheless, a randomized trial should further evaluate the benefit of intense antihypertensive treatment in adults with diabetes.
References
1. Whelton PK, Carey RM, Aronow WS, et al. 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA guideline for the prevention, detection, evaluation, and management of high blood pressure in adults: executive summary: a report of the American College of Cardiology/American Heart Association task force on clinical
practice guidelines. Hypertension. 2018;71:1269–1324. doi:10.1161/HYP.0000000000000066
2. Williams B, Mancia G, Spiering W, et al; ESC Scientific Document Group. 2018 ESC/ESH guidelines for the management of arterial hypertension. Eur Heart J. 2018;39:3021–3104. doi: 10.1093/eurheartj/ehy339
3. de Boer IH, Bangalore S, Benetos A, et al. Diabetes and hypertension: a position statement by the American Diabetes Association. Diabetes Care. 2017;40:1273–1284.
4. Wright JT Jr, Williamson JD, Whelton PK, et al. A randomized trial of intensive versus standard blood-pressure control. N Engl J Med. 2015;373:2103–2116.
5. Lonn EM, Bosch J, López-Jaramillo P, et al; HOPE-3 Investigators. Blood pressure lowering in intermediate-risk persons without cardiovascular disease. N Engl J Med. 2016;374:2009–2020. doi: 10.1056/NEJMoa1600175
6. Adler AI, Stratton IM, Neil HA, et al. Association of systolic blood pressure with macrovascular and microvascular complications of type 2 diabetes (UKPDS 36): prospective observational study. BMJ. 2000;321:412–419.
7. Cushman WC, Evans GW, Byington RP, et al. Effects of intensive blood-pressure control in type 2 diabetes mellitus. N Engl J Med. 2010;362:1575–1585.
8. Patel A, MacMahon S, Chalmers J, et al; ADVANCE Collaborative Group. Effects of a fixed combination of perindopril and indapamide on macrovascular and microvascular outcomes in patients with type 2 diabetes mellitus (the ADVANCE trial): a randomised controlled trial. Lancet. 2007;370:829–840. doi: 10.1016/S0140-6736(07)61303-8