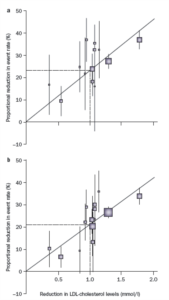
 Body fat distribution and lipids
The past century has witnessed constant progression in the urbanization and industrialization of society, together with automation of labor. This socioeconomic process, referred to as the epidemiological transition, has brought considerable advantages to society. However, high-calorie food has become widely available and fewer calories are burned through physical activity than in the past.16,17 These behavioral changes have led to a dramatic increase in the prevalence of overweight (BMI 25–29.9 kg/m2) and obese (BMI ≥30 kg/m2) individuals over the past few decades.18 The National Health and Nutrition Examination Surveys have shown, in a sample representative of the US population, that the proportion of adults with a BMI of ≥25 kg/m2 rose from 47.0% during the first survey in 1976–1980, to 66.2% in the survey from 2003–2004.19 In parallel, the prevalence of obesity more than doubled from 15.0% to 32.9% during that period.19 Life expectancy has risen slowly, but steadily, over the past two centuries, but evidence now indicates that this increase is reaching a plateau in the USA.20 This trend is likely to be associated with the obesity epidemic. Increases in adiposity indices are primarily seen in young adults aged <20 years, and no evidence indicates a fall in these alarming rates of excess weight and obesity.21,22
Adipose tissue, especially visceral adipose tissue, has an important role in the etiology of insulin resistance and diabetes.23 Visceral adipose tissue is a highly lipolytic endocrine organ that provides a rapid source of energy for peripheral tissues. In conditions of overeating, however, visceral adipose tissue is surrounded by an insulin-resistant and proinflammatory milieu that inhibits the antilipolytic action of insulin, and promotes the hydrolysis of triglycerides and secretion of free fatty acids.22 The increased free fatty acid flux derived from this dysfunctional adipose tissue closely correlates with ectopic accumulation of fat in other tissues, such as the liver, pancreas, heart, and skeletal muscle.23 Although a discussion of the association between visceral adiposity, ectopic fat, and lipids is beyond the scope of this Review,24,25 it should be recognized that a lipid-loaded, or steatotic, liver promotes the secretion of apolipoprotein (apo) B-containing VLDL particles. These particles are cleared slowly by the peripheral organs in individuals who have visceral adiposity and insulin resistance, a condition referred to as the metabolic syndrome.25 Targeting both visceral adiposity and the sedentary lifestyle is of the utmost importance to improve insulin sensitivity and prevent derangements of the lipoprotein–lipid profile that are associated with these prediabetic conditions.26
Although obesity and diabetes do not themselves correlate with variations in levels of LDL cholesterol, they are associated with other parameters of the lipoprotein–lipid and emerging parameters of the lipoprotein–lipid profile and their association with cardiovascular risk are discussed below.
Traditional lipid profiles
The Framingham Heart Study investigators were the first to show that risk of CVD increases as a function of the amount of cholesterol carried by atherogenic lipoprotein subfractions, such as LDL, and is negatively associated with the concentration of cholesterol transported by antiatherogenic lipoprotein subfractions, such as HDL.27 This finding is similar for both sexes, across age groups and various ethnicities. Most risk-score algorithms in clinical practice use levels of total cholesterol or LDL cholesterol and HDL cholesterol as lipid parameters.28,29 However, calculating cardiovascular risk solely on the basis of LDL-cholesterol and HDL-cholesterol levels is an oversimplification, as other lipoprotein subfractions that transport cholesteryl esters in the circulation, such as VLDL, IDL, and chylomicron remnants, are also proatherogenic. The understanding that all cholesteryl esters transported by lipoproteins other than HDL are atherogenic has led to the concept that non-HDL-cholesterol levels (total cholesterol minus HDL cholesterol) might be more strongly associated with CVD risk than LDL-cholesterol levels alone.30 Our group has shown that, even in individuals with low LDL-cholesterol levels (<100 mg/dl), individuals with non-HDL-cholesterol levels of ≥130 mg/dl had a relative risk of future CHD of 1.84 (95% CI 1.12–3.04) compared with those with levels of non-HDL cholesterol of <130 g/dl.31 The fact that non-HDL-cholesterol levels better predict CHD risk than LDL-cholesterol levels in most, if not all, studies could be explained by the idea that non-HDL cholesterol is a better predictor of the number of circulating atherogenic LDL particles than are levels of LDL cholesterol.
In addition to carrying cholesteryl esters, lipoproteins transport other hydrophobic molecules, such as triglycerides. Whereas the predictive value of cholesterol levels depends on the lipoprotein subfraction that it is being carried by, the total concentration of triglycerides is the measure that is positively associated with incidence of CVD.32–34 Although triglycerides are traditionally measured during the fasting state, triglycerides obtained during the postprandial state could in fact be more strongly associated with CVD risk than fasting triglycerides.32–34 Despite the relationship between triglyceride levels and CVD risk, reports have indicated that CVD outcomes might be influenced by correlates of plasma triglyceride levels, such as non-HDL-cholesterol levels, HDL-cholesterol levels, or LDL particle size, making triglycerides a marker of, rather than a risk factor for, CVD and a potential therapeutic target.35 This hypothesis was challenged by a study using Mendelian randomization to explore potential causality.36 This investigation by the Triglyceride Coronary Disease Genetics Consortium and the Emerging Risk Factor Collaboration (ERFC)36 showed that a polymorphism (‑1131T>C [rs662799]) in the promoter of the apo A5 gene (APOA5), which is strongly and consistently associated with plasma levels of triglycerides, was also associated with incident CHD. The fact that this single-nucleotide polymorphism in APOA5 directly affects triglyceride metabolism, and is only indirectly associated with other lipid parameters such as LDL particle size, indicates that triglyceride-mediated pathways might in fact be causally associated with CHD risk.
The likelihood that a cardiovascular event will occur might not be determined solely by atherogenic lipoproteins, but rather by the balance between atherogenic and atheroprotective lipoproteins. Several investigators have shown that the ratio between these particles predicts CVD risk better than isolated lipoprotein subfractions.31,37–39 Therefore, the triglyceride to HDL-cholesterol ratio, and, more importantly, the total cholesterol to HDL-cholesterol (TC/HDL‑C) ratio, are often used to estimate an individual’s cardiovascular risk.31,37–39
Apolipoproteins
Apolipoproteins are found in the phospholipid bilayer of lipoproteins. The composition of the apolipoprotein defines the role and function of the lipoprotein. The principal apolipoprotein on HDL particles is apo A‑I; however, HDL also contains many other components, including apo A-II.40 LDL particles carry apo B as their principal apolipoprotein. Measurement of apolipoprotein concentrations provide a method of quantifying the concentration of lipoproteins, rather than their cholesterol content. Because apo B molecules are not only carried by LDL, but also by other atherogenic lipoproteins such as VLDL and IDL, the concentration of apo B is a more-accurate measure of the total concentration of atherogenic particles than the concentration of LDL cholesterol.41 Decreased LDL particle size is another CVD risk factor that is independent of LDL-cholesterol concentration.42,43 Among individuals carrying an equivalent amount of cholesterol in the LDL subfraction, those with a greater number of small LDL particles have more circulating LDL particles and, therefore, higher levels of apo B. This state is associated with an increased CVD risk independent of LDL-cholesterol levels.42,43 Plasma concentrations of apo B are the best correlate of this state, which could explain the superiority of apo B levels over LDL-cholesterol levels in predicting CVD risk.44 The concentration of apo B is highly correlated with non-HDL-cholesterol levels,45 and these two parameters have been suggested to be interchangeable, although this proposition is not unanimous.46
Although the evidence supporting the cardiovascular benefits of having elevated HDL-cholesterol levels is irrefutable, levels of apo A‑I could also be clinically relevant. In fact, the anti-inflammatory and antioxidant properties of HDL particles are thought by some investigators to be attributable to apo A‑I rather than to the overall number of HDL particles or their cholesterol content.47 However, the number of apo A‑I molecules per HDL particle varies, which renders the counting of HDL particles somewhat difficult on the basis of apo A‑I levels. In most studies, however, the predictive value of apo A‑I is generally equivalent to that of HDL cholesterol.35
As is the case for traditional lipid parameters, the ratio of proatherogenic to antiatherogenic apolipoproteins could be a better estimate of CVD risk than either alone. For apolipoproteins, this relationship is best reflected by the apo B/apo A‑I ratio.48 The Québec Cardiovascular Study49 was one of the first investigations to show that the apo B/apo A‑I ratio is strongly associated with ischemic heart disease (IHD) risk, even among individuals with a low TC/HDL‑C ratio. However, no association between the TC/HDL‑C ratio and risk of IHD in individuals with a low apo B/apo A‑I ratio was reported in this study.49 In the large-scale Apolipoprotein-related MOrtality RIsk Study (AMORIS),50 a strong association between the apo B/apo A‑I ratio and risk of myocardial infarction was observed in more than 175,000 participants. This relationship was independent of the TC/HDL‑C ratio.50 INTERHEART15 was a case–control study comparing 12,461 patients with acute myocardial infarction with 14,637 age-matched and sex-matched controls. This study confirmed that, within each tertile of the TC/HDL‑C ratio, individuals with an elevated apo B/apo A‑I ratio were at increased risk of myocardial infarction. Again, the TC/HDL‑C ratio was not associated with risk of myocardial infarction in the setting of a low apo B/apo A‑I ratio.15 An important aspect of INTERHEART is that the study population is representative of the general population, and that the relationship between the apo B/apo A‑I ratio and risk of myocardial infarction was consistent between males and females and across ethnicities. Similar results from prospective studies have been reported. For example, the International Studies of Infarct Survival (ISIS) Collaborators51 who studied a sample of 3,510 patients with acute myocardial infarction and 9,805 control patients from the UK, have reported that apolipoproteins provide more-useful information on CVD risk than do traditional lipids. In the Women’s Health Study,52 the apo B/apo A‑I ratio had a similar predictive value to non-HDL-cholesterol levels, although these parameters were not directly compared.52 A study conducted by the ERFC showed that the predictive value of non-HDL cholesterol and apo B were very similar, as were the predictive value of HDL cholesterol and apo A‑I.35 Unfortunately, lipid ratios were not reported in this large-scale meta-analysis. In addition, it should be noted that ERFC did not report which of the included studies used unstandardized apolipoprotein measurements, which makes these results difficult to interpret. We believe that future meta-analyses should focus on studies with standardized apolipoprotein measurements. Moreover, although several of the individual studies included in this meta-analysis showed that apo B was more-strongly associated with CHD than non-HDL cholesterol, none of these studies reported the opposite finding. In the Caerphilly Study,53 measurement of traditional lipid parameters were more-closely associated with IHD outcomes than were apolipoproteins.53 However, lipid ratios were not studied, and only a modest number of incident IHD cases (n = 282) were included. Therefore, the relative weight of the ‘negative’ studies is considerably smaller than those supporting the usefulness of apolipoprotein-based lipid ratios.
Although most studies have shown that the apo B/apo A‑I ratio better discriminates CVD risk than standard lipid ratios, whether adding the apo B/apo A‑I ratio to either traditional lipid profiles or CVD risk-prediction algorithms would result in a more-accurate prediction of CVD is unknown. In a nested case–control analysis of the European Prospective Investigation into Cancer and Nutrition (EPIC)-Norfolk study,54 the apo B/apo A‑I ratio was more closely associated with future CHD events than the TC/HDL‑C ratio.54 However, these two lipid ratios were equivalent in their ability to discriminate between individuals who did develop CHD from those who did not. Using a similar approach, the Framingham Heart Study confirmed that the apo B/apo A‑I ratio showed a consistent relationship with CHD risk, but failed to add to a basic risk-prediction model that includes traditional CHD risk factors, such as the TC/HDL‑C ratio.39
Alternative lipoprotein measurements
Nuclear magnetic resonance (NMR) spectroscopy is a method used to measure concentrations of plasma lipoprotein particles in a reagentless manner.55 In addition to measuring the concentrations of lipoprotein subfractions, this technology enables the simultaneous estimation of the size of various lipid subfractions, such as VLDL, IDL, LDL, and HDL.56 The relationship between NMR-measured lipoprotein phenotypes and cardiovascular risk has been investigated in several population-based studies.57 In the Multi-Ethnic Study of Atherosclerosis,58 the concentration of small LDLNMR particles correlated well with the extent of subclinical atherosclerosis, as quantified by carotid intima–media thickness.58 Interestingly, this study showed that, after adjusting for the number of small LDLNMR particles, the number of large LDLNMR particles was positively associated with carotid intima–media thickness, suggesting that all LDL particles are atherogenic regardless of size. In the Women’s Health Study,59 Mora and colleagues investigated the relationship between various lipoprotein phenotypes measured by NMR spectroscopy in a study that included 27,673 women, of whom 1,015 developed CVD during the follow-up of 11 years. With the exception of the number of large LDLNMR particles, all atherogenic NMR-related lipoprotein concentrations were significantly associated with cardiovascular risk (P <0.001). The number of LDLNMR particles showed the strongest association with CVD risk (relative risk of incident CVD comparing the top versus bottom quintile was 2.51 [95% CI 1.92–3.30]). Only the number of large HDLNMR particles as well as mean HDL particle size were associated with a reduced CVD risk.59 We have reported that HDL-cholesterol levels, the total concentration of HDL particles (HDLNMR), as well as HDL particle size were all negatively associated with the risk of developing CHD in men and women in the EPIC-Norfolk study population.60 In this study, we also found that the relationship between both HDL-cholesterol levels and HDL particle size and CVD risk was almost irrelevant after adjusting for some components of the metabolic syndrome, including apo B and triglyceride levels. However, the strong relationship between the concentration of HDL particles and CHD risk was not affected upon adjusting for these features of the metabolic syndrome.60
To date, NMR spectroscopy has been used in only two prospective studies to compare cholesterol-based, apolipoprotein-based, and NMR-based lipoprotein ratios in the prediction of cardiovascular risk.59,61 In the Women’s Health Study,59 the TC/HDL‑C and apo B/apo A‑I ratios were strongly and similarly associated with CVD risk, whereas the relationship between the LDLNMR/HDLNMR ratio and cardiovascular risk was statistically significant yet of a lesser magnitude. Interestingly, we have reported very similar results for women enrolled in the EPIC-Norfolk study.61 All three lipid ratios were also strongly and similarly associated with CHD risk in men.
The physicochemical properties of lipoproteins, such as decreased particle size or increased particle density, are associated with CVD risk.42,43,62 However, the association between LDL or HDL particle size and CVD risk is generally not independent of traditional lipid profiles. The particle size of a lipoprotein can be reliably measured by both gradient gel electrophoresis and NMR spectroscopy, although lipoprotein size measured by the latter could be more closely associated with coronary risk.63 Berkeley HeartLab (San Francisco, CA, USA) have developed a diagnostic test (LDL‑S3GGE®) that estimates the mean LDL particle size based on the migration distance of seven predetermined LDL subclasses. Multiplication of the relative distribution of these subclasses by apo B concentration can provide a quantitative volume (in mg/dl) of LDL subclasses. This concept is based on the same principles as NMR spectroscopy, but uses physical rather than chemical separation of LDL subclasses. Although we think this approach could be cost-effective, the absence of studies associating LDL subclasses with CVD risk is a major limitation.
The Vertical Auto Profile test from Atherotech (Birmingham, AL, USA) has been used in a number of clinical trials to evaluate changes in LDL or HDL subclasses following lipid-lowering therapy.64,65 This test separates lipoprotein subclasses according to their density using vertical spin density gradient ultracentrifugation.66 Similar to gradient gel electrophoresis and NMR spectroscopy, this test is not routinely used in the clinical setting as no solid evidence exists that this test could be clinically useful over and above cholesterol-based or apolipoprotein-based measurements.
Lipoprotein(a)Lipoprotein(a) (Lp[a]) is an LDL-like particle, where an apo(a) is covalently bound to the apo B molecule. Two meta-analyses have shown that Lp(a) concentration, as well as the various apo(a) isoforms, are associated with CVD risk, and that these associations are consistent, yet modest.67,68 By assessing single-nucleotide polymorphisms in candidate genes selected for their potential relevance to CVD, the investigators of the Precocious Coronary Artery Disease (PROCARDIS) study69 have shown that the LPA locus on 6q26–27 encoding apolipoprotein(a) has a strong association with both Lp(a) levels and CVD risk; however, this relationship is attenuated upon adjustment for Lp(a) levels. A strong and positive association between genetically elevated Lp(a) levels and myocardial infarction risk has also been reported by the investigators of the Copenhagen City Heart Study.70 The European Atherosclerosis Society was the first organization to recommend screening for elevated concentrations of Lp(a).71 The consensus panel suggested that individuals with elevated Lp(a) levels could be treated with niacin, although the panel acknowledged that no randomized, controlled trial data currently support this approach (Box 1).
Lipoprotein-associated phospholipase A2
Lipoprotein-associated phospholipase A2 (Lp-PLA2) is an enzyme that binds to LDL and hydrolyzes the sn‑2-acyl bond of phospholipids in cell membranes and lipoproteins. This process yields nonesterified fatty acids and lysophospholipids, which are precursors of several proinflammatory mediators.72 Lp-PLA2 also has an important role in lipid remodeling by binding to the electronegative domains of small, dense LDL particles and apo B.72 Plasma levels and activity of Lp-PLA2 have been shown to be positively associated with cardiovascular risk.73 A phase III study evaluating the effect of the Lp-PLA2 inhibitor darapladib on cardiovascular outcomes is ongoing, so questions regarding the potential clinical relevance of Lp-PLA2 should be answered in the upcoming years.74 A trial testing the efficacy of varespladib (an inhibitor of secretory PLA2) in reducing
cardiovascular outcomes is also being conducted.7 |

