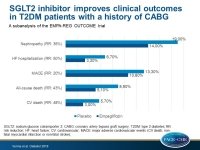
SGLT2 inhibitor improves clinical outcomes in T2DM patients with a history of coronary artery bypass graft surgery
In type 2 diabetic patients with a history of CABG, empagliflozin reduced significantly CV- and all-cause mortality, HF hospitalization, and incident or worsening nephropathy compared with placebo.
Empagliflozin reduces cardiovascular events, mortality and renal events in participants with type 2 diabetes after coronary artery bypass graft surgery: subanalysis of the EMPA-REG OUTCOME® randomised trialLiterature - Verma S, Mazer D, Fitchett D, et al. - Diabetologia 2018; published online ahead of print
Introduction and methods
Patients with type 2 diabetes (T2DM) and a history of coronary artery bypass graft (CABG) surgery have an increased CV risk, with a 5-year event rate up to 29% for major adverse CV events (MACE) [1,2]. In this analysis of the EMPA-REG OUTCOME trial [3], the effect of empagliflozin on CV outcomes and mortality was evaluated in the subgroup of T2DM patients with a self-reported history of CABG at baseline.
The EMPA-REG OUTCOME trial evaluated the CV safety of empagliflozin (10 mg or 25 mg) versus placebo in patients with T2DM and established CVD on top of standard of care therapy. Overall, empagliflozin led to a 38% reduction in CV mortality, a 32% reduction in all-cause mortality, a 35% reduction in HF hospitalization, and a 39% reduction in incident or worsening nephropathy, compared with placebo. The primary outcome was a composite of CV death, non-fatal myocardial infarction and non-fatal stroke (MACE).
In T2DM patients with a history of CABG, the following outcomes were assessed during a median observation time of 3.1 years: MACE, CV death, all-cause death, hospitalization for heart failure (HF), as well as incident or worsening nephropathy.
Main results
Out of 7020 participants, 25% in the empagliflozin group and 24% in the placebo group had a history of CABG. In this subgroup, compared with placebo, empagliflozin was associated with:
- a 48% reduction in the risk of CV death (3.0% vs. 5.7%; HR: 0.52; 95%CI: 0.32- 0.84)
- a 43% reduction in the risk of all-cause mortality (5.1% vs. 8.9%; HR: 0.57; 95%CI: 0.39-0.83)
- a 20% reduction in the risk of MACE (10.6% vs. 13.3%; HR: 0.80; 95%CI: 0.60-1.06)
- a 50% reduction in the risk of HF hospitalization (3.3% vs 6.7%; HR: 0.50; 95%CI: 0.32-0.77)
- a 35% reduction in the risk of incident or worsening nephropathy (14.0% vs. 19.0%; HR: 0.65; 95%CI: 0.50-0.84)
There were no significant differences between participants with and without a history of CABG at baseline (P>0.05 for treatment by subgroup interactions).
The risk of myocardial infarction, stroke, serious adverse events or adverse events leading to drug discontinuation was similar between the empagliflozin and placebo group.
Conclusion
In patients with T2DM and a history of CABG, empagliflozin on top of standard of care was associated with significant reductions in CV- and all-cause mortality, HF hospitalization, and incident or worsening nephropathy, compared with placebo. The authors suggest that empagliflozin should be considered as secondary prevention after CABG surgery in T2DM patients to reduce the risk of MACE and mortality.
References
1. Farkouh ME, Domanski M, Sleeper LA et al (2012) Strategies for multivessel revascularization in patients with diabetes. N Engl JMed 367:2375–2384
2. Kappetein AP, Head SJ, Morice MC et al (2013) Treatment of complex coronary artery disease in patients with diabetes: 5-year results comparing outcomes of bypass surgery and percutaneous coronary intervention in the SYNTAX trial. Eur J Cardiothorac Surg 43:1006–1013
3. Zinman B,Wanner C, Lachin JM et al (2015) Empagliflozin, cardiovascular outcomes, and mortality in type 2 diabetes. N Engl J Med 373:2117–2128