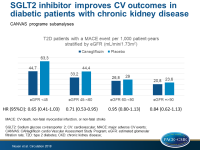
SGLT2 inhibitor improves CV and renal outcomes in diabetic patients with chronic kidney disease
In type 2 diabetes patients at high CV risk and chronic kidney disease, the SGLT2 inhibitor canagliflozin consistently improved CV and renal outcomes across different levels of kidney function.
Cardiovascular and Renal Outcomes With Canagliflozin According to Baseline Kidney Function: Data from the CANVAS ProgramLiterature - Neuen BL, Ohkuma T, Neal B, et al. - Circulation 2018; published online ahead of print
Introduction and methods
Sodium glucose co-transporter 2 (SGLT2) inhibitors are associated with improvements in glycemic status, blood pressure, weight, and proteinuria in patients with type 2 diabetes (T2DM) [1]. However, SGLT2 inhibitors are not recommended for T2DM patients with impaired kidney function [2].
In this post hoc analysis of the CANagliflozin cardio Vascular Assessment Study Program (CANVAS) [3], the effect of the SGLT2 inhibitor canagliflozin on CV, renal, and safety outcomes was assessed, in patients with T2DM at high CV risk and chronic kidney disease (CKD) at different levels of kidney function, including those for whom canagliflozin is currently not approved (estimated glomerular filtration rate [eGFR]: 30-45 mL/min/1.73m2).
The CANVAS Program included two double-blind, placebo-controlled, randomized trials (CANVAS and CANVAS-R) that evaluated the CV and renal safety and efficacy of canagliflozin in T2DM patients with established CVD or at high CV risk. Patients with eGFR <30 mL/min/1.73m2 were excluded from the study. Patients were randomized to receive either canagliflozin 100-300 mg daily, or placebo.
The primary endpoint was the composite of CV death, non-fatal myocardial infarction (MI), or non-fatal stroke. The main renal endpoint was the composite of end-stage kidney disease, renal death, and a 40% decrease in eGFR, or a doubling of serum creatinine. The mean follow-up was 188.2 weeks. Analyses were done using eGFR categories of <45, 45-<60, 60-<90, ≥90 mL/min/1.73m2.
Main results
- Out of 10,142 T2DM patients, 20.1% had CKD at baseline, including 554 (5.5%) with an eGFR <45 mL/min/1.73m2.
- The placebo-adjusted mean difference in glycated hemoglobin was -0.76% in patients with baseline eGFR ≥90 mL/min/1.73m2, -0.57% in those with baseline eGFR 60-<90 mL/min/1.73m2, -0.45% in those with baseline eGFR 45-<60 mL/min/1.73m2, and -0.35% in patients with eGFR<45 mL/min/1.73m2 (Pheterogeneity <0.0001).
- The primary outcome was similarly reduced independently of eGFR subgroup (HR: 0.65; 95%CI: 0.41-1.03 for eGFR <45 mL/min/1.73m2, HR: 0.71; 95%CI: 0.53-0.95 for eGFR 45-<60 mL/min/1.73m2, HR: 0.95; 95%CI: 0.80-1.13 for eGFR 60-<90 mL/min/1.73m2, HR: 0.84; 95%CI: 0.62-1.13 for eGFR ≥90 mL/min/1.73m2, Pheterogeneity =0.33). There was heterogeneity for fatal/non-fatal stroke, in favor of declining kidney function (HR: 0.87; 95%CI: 0.69-1.09; Pheterogeneity=0.01).
- The HRs for the main renal endpoint favored canagliflozin vs placebo in all eGFR subgroups (HR: 0.65; 95%CI: 0.29-1.48 for eGFR <45 mL/min/1.73m2, HR: 0.78; 95%CI: 0.46-1.31 for eGFR 45-<60 mL/min/1.73m2, HR: 0.58; 95%CI: 0.41-0.84 for eGFR 60-<90 mL/min/1.73m2, HR: 0.44; 95%CI: 0.25-0.78 for eGFR ≥90 mL/min/1.73m2).
- In the first 13 weeks of the study, all eGFR subgroups had a decline in eGFR (placebo-subtracted differences: -1.89 for eGFR ≥90 mL/min/1.73m2, -2.33 for eGFR 60-<90 mL/min/1.73m2, -2.85 for eGFR 45-<60 mL/min/1.73m2, -2.75 for eGFR <45 mL/min/1.73m2), whereas from week 13 to the end of follow-up, the decline in kidney function was significantly slowed in all subgroups (placebo-subtracted mean slope differences: 1.47, 1.09, 1.05, 1.35 mL/min/1.73m2 per year respectively).
- Relative effects on safety outcomes were similar across eGFR subgroups after canagliflozin treatment, with the exception of a borderline significant interaction for hypoglycemia in the four eGFR subgroups (Pheterogeneity=0.06).
Conclusion
In T2DM patients with established CVD or at high CV risk and CKD, canagliflozin consistently improved renal and CV outcomes across different levels of kidney function down to eGFR 30 mL/min/1.73m2 . Current eGFR-based limitations may be reconsidered for prescription of canagliflozin to those with impaired kidney function.
References
1. Heerspink HJ, perkins BA, Fitchett DH, et al. Sodium glucose cotransporter 2 inhibitors in the treatment of diabetes mellitus: cardiovascular and kidney effects, potential mechanisms, and clinical applications. Circularion 2016;134:752-772.
2. Scheen AJ. Pharmacokinetics, pharmacodynamics and clinical use of SGLT2 inhibitors in patients with type 2 diabetes mellitus and chronic kidney disease. Clin Pharmacokinet 2015;54:691-708.
3. Neal B, Perkovic V, Mahaffey KW, et al. Canagliflozin and cardiovascular and renal events in type 2 diabetes. N Engl J Med 2017;377:644-657.